Analysis Of Published Papers
In the past decade, the total number of papers on depression published worldwide has increased year by year as shown in Fig. 1A. Searching the Web of Science database, we found a total of 43,863 papers published in the field of depression from 2009 to 2019 or ts = ) and py = , Articles). The top 10 countries that published papers on the topic of depression are shown in Fig. 1B. Among them, researchers in the USA published the most papers, followed by China. Compared with the USA, the gap in the total number of papers published in China is gradually narrowing , but the quality gap reflected by the index is still large, and is lower than the global average . As shown in Fig. 1E, the hot research topics in depression are as follows: depression management in primary care, interventions to prevent depression, the pathogenesis of depression, comorbidity of depression and other diseases, the risks of depression, neuroimaging studies of depression, and antidepressant treatment.
Fig. 1
Analysis of published papers around the world from 2009 to 2019 in depressive disorder. A The total number of papers . B The top 10 countries publishing on the topic. C Comparison of papers in China and the USA. D Citations for the top 10 countries and comparison with the global average. E Hot topics.
Deterrence And Patient Education
Patient education has a profound impact on the overall outcome of major depressive disorder. Since MDD is one of the most common psychiatric disorders causing disability worldwide and people in different parts of the world are hesitant to discuss and seek treatment for depression due to the stigma associated with mental illness, educating patients is very crucial for their better understanding of the mental illness and better compliance with the mental health treatment. Family education also plays an important role in the successful treatment of MDD.
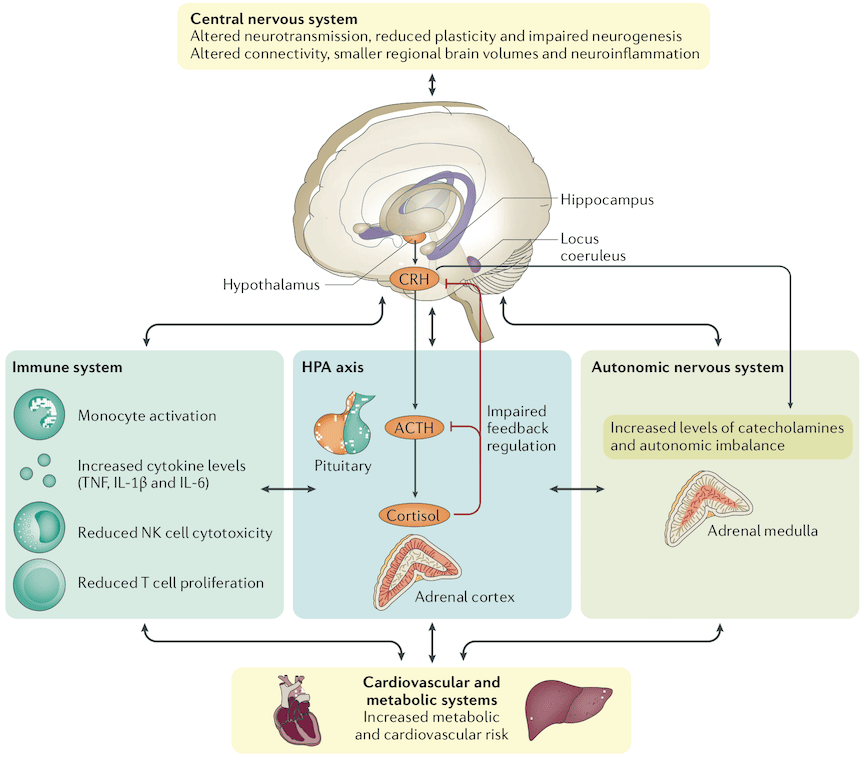
The Immune System And Inflammation
Of relevance is the question as to whether patients with major depression are more likely to be infected with bacteria or viruses when compared with the general population. There is considerable evidence that a past history of major depression is associated with an increased risk of infections, and this is generally interpreted to mean that patients with major depression are relatively immunosuppressedand this in spite of the observed increase in proinflammatory cytokines. A related and relatively unexplored area is the relationship of major depression to autoimmune disease, alluded to earlier in this review. This bidirectional relationship is now well established. Patients with major depression have an increased risk of developing autoimmune diseases such as systemic lupus erythematosus, rheumatoid arthritis, autoimmune thyroiditis, multiple sclerosis, and irritable bowel syndrome, and patients with these disorders have high rates of major depression .
As in the discussion above on brain imaging, the role of childhood maltreatment in the inflammation observed in patients with major depression is of paramount consideration. There is much evidence, preclinical and clinical, that early-life trauma results in a long-lasting increase in proinflammatory cytokine secretion .
You May Like: Is Depression And Anxiety A Mental Illness
Personalized Medicine In Depression Treatment
In addition to pharmacogenomics, the other two major areas that have been explored as putative indices of treatment response in major depression are brain imaging and EEG. Space constraints preclude any serious review of the former area, but it is clear that functional connectivity studies, including those noted in an earlier section and others, such as that based on the 1,000-patient International Study to Predict Optimized Treatment in Depression , hold great promise. As regards EEG, as recently as 2019, the APA Work Group on Biomarkers and Novel Treatments reviewed the literature and concluded that the available evidence did not support EEG as a reliable predictor of antidepressant use .
However, two recent reports lend support to the notion that more advanced analytic techniques applied to EEG data provide strong support for rethinking this conclusion. Wu et al. studied 309 patients with major depression in the Establishing Moderators and Biosignatures of Antidepressant Response for Clinical Care for Depression study and identified predictions of sertraline response. This was confirmed in two replication samples. More recently, Zhdanov et al. , using a machine-learning approach in 122 patients treated with escitalopram, found that baseline EEG recordings identified the SSRI responders with accuracy of almost 80% . For those patients in whom EEG was obtained at week 2 of treatment, the prediction was even better.
Brain Imaging And Neuroimaging Studies
Neuroimaging, including magnetic resonance imaging and molecular imaging, provides a non-invasive technique for determining the underlying etiology and individualized treatment for depression. MRI can provide important data on brain structure, function, networks, and metabolism in patients with depression it includes structural MRI , functional MRI , diffusion tensor imaging, and magnetic resonance spectroscopy.
Diffusion tensor imaging detects the microstructure of the white matter, which has been reported impaired in patients with depression . A recent meta-analysis that included first-episode and drug-naïve depressive patients showed that the decrease in fractional anisotropy was negatively associated with illness duration and clinical severity .
fMRI, including resting-state and task-based fMRI, can divide the brain into self-related regions, such as the anterior cingulate cortex, posterior cingulate cortex, medial prefrontal cortex, precuneus, and dorsomedial thalamus. Many previous studies have shown the disturbance of several brain areas and intrinsic neural networks in patients with depression which could be rescued by antidepressants . Further, some evidence also showed an association between brain network dysfunction and the clinical correlates of patients with depression, including clinical symptoms and the response to antidepressants , ECT , and repetitive transcranial magnetic stimulation .
Table 1. Findings of the ENIGMA Consortium.
Recommended Reading: How Can I Get Out Of Depression Without Drugs
Genes And Psychosocial Stress
Family, twin, and adoption studies provide very solid and consistent evidencethat MDD is a familial disorder and that this familiality is mostly or entirelydue to genetic factors 4. This importantfinding suggests that parental social behavior and other familial environmentalrisk factors are not as important in the pathogenesis of MDD as previouslyassumed and should not be the major focus of the treatment of the disorder.
The above-mentioned studies consistently show that the influence of geneticfactors is around 30-40% 4. Non-geneticfactors, explaining the remaining 60-70% of the variance in susceptibilityto MDD, are individual-specific environmental effects . These effects are mostlyadverse events in childhood and ongoing or recent stress due to interpersonaladversities, including childhood sexual abuse, other lifetime trauma, lowsocial support, marital problems, and divorce 5,6.
These results suggest that there is a huge potential in the preventionof MDD by means of psychosocial interventions .In addition, these results mirror the clinical practice of empirically validatedpsychotherapies to treat depression 7,8,9,including interpersonal, psychodynamic and cognitive behavioral psychotherapiesand cognitive behavioural analysis system of psychotherapy, which all focusdirectly or indirectly on interpersonal difficulties and skills. This doesnot exclude the fact that unidentified non-genetic, non-psychosocial riskfactors may also play important roles in some patients .
What Happened To The Monoamine Theory Of Depression
Unfortunately, the monoamine theory as described has not stood up to close scrutiny. For example, reserpine, which depletes the brain of 95% of serotonin, dopamine, and norepinephrine, produces depression in only about 15% of subjects. If monoamines are that important in mood regulation, how can one walk around with < 5% of ones monoamines and be euthymic? Second, the pharmacological effects of selective serotonin reuptake inhibitors and serotonin-norepinephrine reuptake inhibitors as antagonists at the monoamine transporter sites are immediate, yet their antidepressant effects are delayed for 35 weeks, and even longer in some patients. Third, reappraisal of the biochemical marker studies noted above identified many negative studies that revealed no alterations in indices of activity of these monoamine circuits in depressed patients. Fourth, some antidepressants clearly do not act as reuptake inhibitors at these sites, including bupropion, agomelatine, ketamine, pimavanserin, and others. Fifth, even in previously untreated patients with major depression, SSRIs and SNRIs achieve remission in no more than 50% of the population. Sixth, recent studies by our group have revealed no relationship between serotonin and norepinephrine transporter occupancy and treatment response in previously untreated patients with major depression who received escitalopram or duloxetine.
Recommended Reading: Who Can I Talk To About My Anxiety And Depression
Symptoms Of Major Depressive Disorder
These are some of the symptoms of major depressive disorder you may experience:
- Feeling sad or low
- Having difficulty paying attention, remembering, or making decisions
- Having difficulty sleeping, waking up too early, or oversleeping
- Experiencing unplanned changes in eating habits and weight
- Experiencing headaches, cramps, digestive issues, or other aches and pains that dont have a clear cause and dont get better with treatment
- Talking about death, having thoughts of suicide, or attempting self-harm
Everyone experiences depression differently. While some people may have a few symptoms, others may have many. The frequency, severity, and duration of the symptoms can also vary from person to person.
Treating Major Depressive Disorder
While depression is a serious condition, it can be treated. In fact, between 80% to 90% of people with depression respond well to treatment, and almost all patients get some relief from their symptoms.
Its important to seek treatment for depression as soon as possible, because the earlier it is treated, the more effective the treatment can be. Ignoring the symptoms of depression and leaving it untreated can lead to self-harm or death.
Treatment for depression may involve medication, therapy, or brain stimulation. The treatment modalities chosen can depend on the severity of the depression and your individual needs.
You May Like: Major Depressive Disorder Dsm 5
Nutrition Counseling To Treat Major Depressive Disorder
Nutrition counselors help patients understand how food choices affect mood and energy levels. They teach patients to eat healthy foods that provide the best nutrition for better cognitive functioning.
This type of treatment is called nutritional therapy. For example, a diet rich in fruits and vegetables may help with depressive episodes.
Cognitive Therapy For Depression
Cognitive therapy is highly regarded as psychological therapy. In cognitive therapy, patients learn to challenge their negative beliefs and supplant them with constructive thoughts.
In addition, they are taught to recognize their automatic thoughts and to question their validity.
There is a spectrum of CBTs, including individual and group treatment therapies.
Recommended Reading: I Think I Need Depression Medication
Pathophysiology Of Patients With Depression Versus Healthy Volunteers
Patients With First Episode Depression
All patients and their respective control group were Brazilian and young adults . The majority of the sample were women , in an undergraduate course and with low income . The average patient had depression levels of mild severity . One patient had a comorbid anxiety disorder . Patients showed worse sleep quality than controls and had similar BMI .
Among the sociodemographic characteristics, the Boruta algorithm showed that only age was relevant for discrimination between MD and CG1 groups .
Figure 1. Importance of sociodemographic characteristics for discrimination of patients from controls. The random forestbased algorithm of sociodemographic characteristics relevant to discrimination of: patients with first episode of major depression and the control group . Patients with treatment-resistant major depression and the respective control group . The colors used in the images denote: green, relevant characteristic yellow, tentative of relevance red, no relevant characteristic and blue, randomly shuffled data at a maximum, mean, and minimum levels.
Patients With Treatment-Resistant Depression
Similar Articles Being Viewed By Others
Carousel with three slides shown at a time. Use the Previous and Next buttons to navigate three slides at a time, or the slide dot buttons at the end to jump three slides at a time.
15 July 2020
Wessel A. van Eeden, Albert M. van Hemert, Erik J. Giltay
10 May 2022
Britta Stapel, Daniela Fraccarollo, Kai G. Kahl
28 September 2021
Federica Klaus, Karoline Guetter, Stefan Kaiser
volume 5, page e649
Recommended Reading: I Am Very Very Depressed
Genetics Epigenetics And Gene
This is a large literature, and I will only briefly discuss the major issues in the field. The seminal question remains that of understanding the discrepancy between the clear findings that approximately one-third of the risk for major depression is genetic and the absence of identification of the genetic substrates that mediate this risk. Genome-wide association studies have attempted, in relatively large samples, to identify the loci that confer risk for major depression. The results have largely been disappointing on two counts. First, in early studies, there appeared to be overlap in risk for major depression and both bipolar disorder and schizophrenia . Second, each of the gene variants identified, although statistically significant because of the large number of subjects studied, alone exerts a very small effect in terms of vulnerability to major depression. Third, unlike schizophrenia and autism spectrum disorder, the identification of copy number variants or rare variants of large effect by exome sequencing in major depression has not been as robust as expected .
We are surely in our infancy in understanding the relative roles of these genetic and epigenetic alterations on relevant molecular mechanisms that involve the synthesis of critical proteins, including receptors, transporters, and enzymes.
Causes Of Major Depressive Disorder
Depression is caused by an imbalance of chemicals, known as neurotransmitters, in the brain.
Certain genetic, biological, psychological, and environmental factors can increase the chances of someone developing depression however, its important to remember that anyone can develop depression.
The potential causes and risk factors for depression include:
You May Like: Angry All The Time Depression
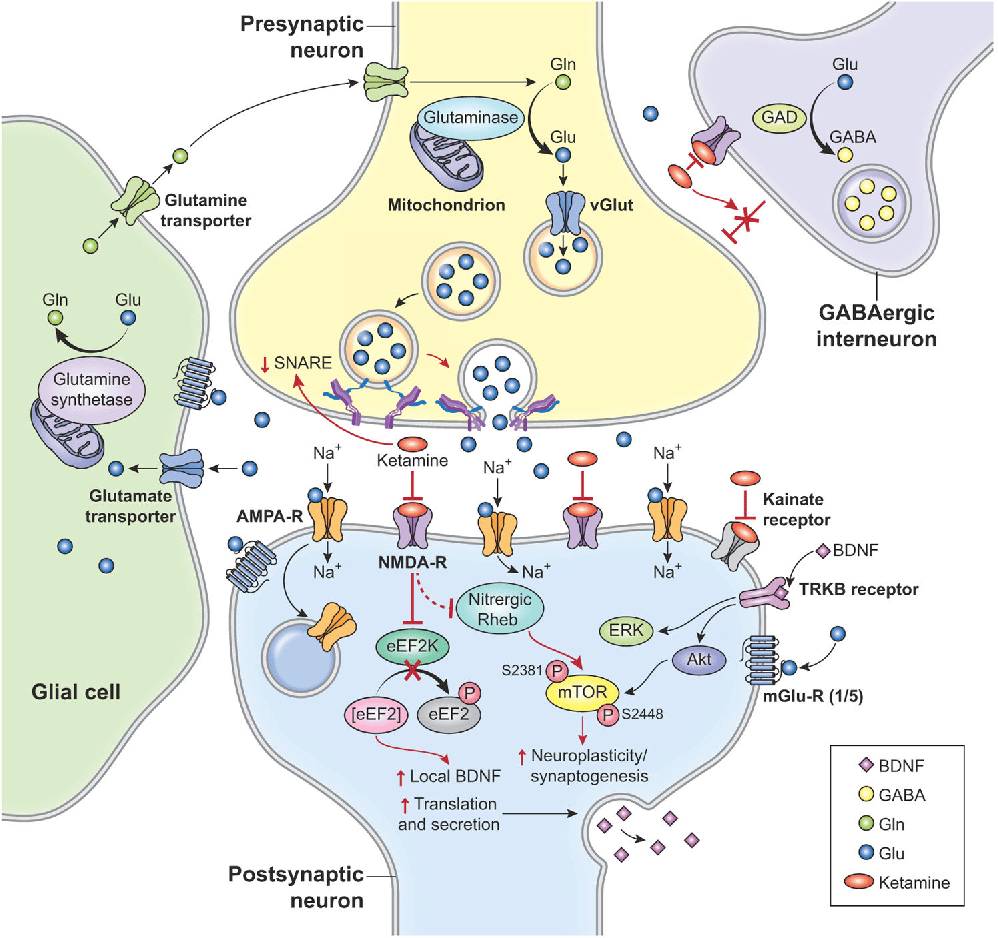
The Neurotrophic Hypothesis Of Depression
Risk factors for depressive episodes change during the course of the illness.The first depressive episode is usually âreactiveâ, i.e., triggeredby important psychosocial stressors, while subsequent episodes become increasinglyâendogenousâ, i.e., triggered by minor stressors or occurringspontaneously 70. There is consistentevidence that the volume loss of the hippocampus and other brain regions isrelated to the duration of depression 71,suggesting that untreated depression leads to hippocampal volume loss, possiblyresulting in increased stress sensitivity 72 andincreased risk of recurrence 73.
Glucocorticoid neurotoxicity, glutamatergic toxicity, decreased neurotrophicfactors, and decreased neurogenesis have been proposed as possible mechanismsexplaining brain volume loss in depression. There is no solid evidence onany of these mechanisms, since there are no imaging tools to directly examineneurotoxic and neurotrophic processes in vivo. Brain derived neurotrophicfactor has attracted considerable interest. Specifically, preclinicalstudies have shown correlations between stress-induced depressive-like behaviorsand decreases in hippocampal BDNF levels, as well as enhanced expression ofBDNF following antidepressant treatment 74.The clinician should be aware of the potentially brain-damaging effect ofdepression and treat depressed patients as early and effectively as possible.
Finding The Mdd Therapy You Need
Major depressive disorder affects millions of Americans each year.
Fortunately, many effective treatments are available today, including combined treatment methodologies.
At Neuro Spa Therapy Centers, we offer a variety of treatments to suit the needs of each individual patient. If you believe youve been suffering from major depressive disorder, book a free consultation with us today.
This blog post is meant to be educational in nature and does not replace the advice of a medical professional. See full disclaimer.
Also Check: Medical Leave For Depression And Anxiety
Drug Therapy For Depression
Several drug classes and drugs can be used to treat depression:
Choice of drug Drug Choice and Administration of Antidepressants Several drug classes and drugs can be used to treat depression: Selective serotonin reuptake inhibitors Serotonin modulators Serotonin-norepinephrine reuptake inhibitors… read more may be guided by past response to a specific antidepressant. Otherwise, SSRIs are often the initial drugs of choice. Although the different SSRIs are equally effective for typical cases, certain properties of the drugs make them more or less appropriate for certain patients .
Enhancing Healthcare Team Outcomes
An interdisciplinary approach is essential for the effective and successful treatment of MDD. Primary care physicians and psychiatrists, along with nurses, therapists, social workers, and case managers, form an integral part of these collaborated services. In the majority of cases, PCPs are the first providers to whom individuals with MDD present mostly with somatic complaints. Depression screening in primary care settings is very imperative. The regular screening of the patients using depression rating scales such as PHQ-9 can be very helpful in the early diagnosis and intervention, thus improving the overall outcome of MDD. Psychoeducation plays a significant role in improving patient compliance and medication adherence. Recent evidence also supports that lifestyle modification, including moderate exercises, can help to improve mild-to-moderate depression. Suicide screening at each psychiatric visit can be helpful to lower suicide incidence. Since patients with MDD are at increased risk of suicide, close monitoring, and follow up by mental health workers becomes necessary to ensure safety and compliance with mental health treatment. The involvement of families can further add to a better outcome of the overall mental health treatment. Meta-analyses of randomized trials have shown that depression outcomes are superior when using collaborative care as compared with usual care.
Recommended Reading: Anti Depression Meds For Weight Loss
Physical And Mental Comorbidities Of Mdd
MDD is associated with poorer physical health, including high comorbidity with chronic physical conditions and higher rates of disability. There are multiple mechanisms by which physical conditions can predispose individuals to MDD. The traumatic experience of illness and the dysfunction that comes with it can trigger a depressive episode.100100. Helgeson VS, Zajdel M. Adjusting to chronic health conditions. Annu Rev Psychol. 2017 68:545-71. Biological factors can also be involved: modified inflammatory pathways and immune system changes have been implicated in the pathogenesis of depression,101101. Miller AH, Maletic V, Raison CL. Inflammation and its discontents: the role of cytokines in the pathophysiology of major depression. Biol Psychiatry. 2009 65:732-41. and depression has a pro-inflammatory effect. This could result in a two-way relationship between depression and physical condition.102102. Carney RM, Freedland KE, Miller GE, Jaffe AS. Depression as a risk factor for cardiac mortality and morbidity: a review of potential mechanisms. J Psychosom Res. 2002 53:897-902.
Finally, some limitations should be addressed. Since most of the included studies were cross-sectional, causal relationships could not be established. The risk factor studies had heterogeneous methodologies, which impedes comparison of the results. Additionally, in retrospective studies there may be a recall bias regarding traumatic experiences.