Approvals Inclusion And Exclusion Criteria
We included subjects who experienced 2 previous MDD-episodes according to the structured clinical interview for Diagnostic and Statistical Manual of Mental Disorders, fourth edition diagnoses , but were in stable remission 7 , and not currently in an MDD-episode . Participants were 3565 years, to include a homogeneous age group and minimize the risk of later conversion to bipolar disorder. Second, we included never-depressed controls without personal psychiatric history by SCID-analysis, or first-degree familial psychiatric history, matched to the rrMDD subjects for age, sex, educational level, working class and ethnicity. Both groups were recruited using identical advertisements in freely available sources and from previous studies. This study was approved by the accredited Academic Medical Centre Medical Ethical Committee , and conformed to the Declaration of Helsinki. Eleven of 40 healthy control females and 7 out of 19 healthy control males were recruited at the University of California, San Diego under IRB-approved protocol #140072 with signed informed consent. We excluded subjects with current diagnoses of alcohol and/or drug dependence, psychotic or bipolar symptoms, predominant anxiety or severe personality disorder. Other exclusion criteria included standard MRI-exclusion criteria, history of severe head trauma or neurological disease, or severe general physical illness. All participants had to be without psychoactive medication for 4 weeks.
Diagnosis Specificity Goes Beyond Reimbursement In This Case Supporting Documentation And The Further Specified Diagnosis Lets Everyone Else Know The Patients Acuity
You review the PHQ-9 questionnaire and see a score of 25. In your note, you document the patients symptoms along with a diagnosis of depression make a referral for follow up care start the patient on an antidepressant to help with the symptoms and schedule a follow up visit in 3 weeks to assess the effectiveness of the medication.
It looks like you covered all your bases, but before you close out that chart, pause for a minute and consider the following questions:
Did you know Depression codes to Depression, Unspecified and does not reflect the severity or episode of the disorder?
- Does your diagnosis accurately reflect the acuity or severity of depression for the patient?
- Does the diagnosis reflect the resources a care coordination team may utilize to make sure the patient receives the appropriate follow up care or interventions?
- Does the diagnosis support the need for a referral or the medication you prescribed?
- Does the diagnosis of depression support the E/M level of service?
- Is a treatment plan, pharmacotherapy, and/or psychotherapy recommended on the PHQ-9 for a diagnosis of depression?
Symptoms Of Major Depressive Disorder And Their Impact On Psychosocial Functioning In The Different Phases Of The Disease: Do The Perspectives Of Patients And Healthcare Providers Differ
- 1Medical Affairs, H. Lundbeck A/S, Valby, Denmark
- 2Biostatistics, Lundbeck Singapore Pte. Ltd., Singapore, Singapore
- 3Department of Psychiatry and Psychotherapy, University of Münster, Münster, Germany
- 4Department of Psychiatry, Melbourne Medical School, University of Melbourne, Melbourne, VIC, Australia
- 5The Florey Institute of Neuroscience and Mental Health, University of Melbourne, Melbourne, VIC, Australia
Don’t Miss: How Do Doctors Test You For Depression
What Residual Symptoms Might Patients With Ir Have
What symptoms might clinicians expect to see in patients who are getting better but still have IR? Common residual symptoms include low mood, anxiety, irritability, guilt, and somatic symptoms.14 While irritability is especially problematic for patients psychosocially, anxiety tends to make remission even more challenging.15 Further, a STAR*D trial16 looked at the types and frequency of residual symptoms in patients who met criteria for remission . Among remitters, over 90% had at least 1 residual symptom the most common symptoms were weight gain and insomnia .
AV 2. Residual Symptoms in Patients With DepressionData from Nierenberg et al.16Abbreviation: QIDS-SR16=16-item Quick Inventory of Depressive Symptomatology, Self-Report.
Ial Remission And Residual Symptoms

Our attention was first drawn to the importance of residual symptoms in a longitudinal follow-up of remission and relapse in depressed patients treated in Cambridge in the early 1990s.- A sample of 64 depressed patients meeting the Research Diagnostic Criteria for definite primary unipolar major depression was identified on presentation, and followed to remission, or for 15 months. Only 4 subjects in the sample of 64 failed to remit to the criterion of 2 months below definite major depression by this point. However, on examining the findings in more detail, although the majority of remitters scored in the lower ranges of the 17-item Hamilton Depression Rating Scale, an important proportion of 32% scored 8 or more on the Hamilton scale, the criterion proposed by Frank et al as indicating full remission or recovery. They spanned a range from 8 to 1 8, although they did not satisfy the criteria for major depression.
Also Check: How To Tell If Someone Is Hiding Depression
Predictors Of Residual Symptoms
Attempts to define predictors of partial and full response to antidepressant therapies have yielded conflicting results in terms of baseline severity,,, personality traits, and the impact of life events.,, Paykel’s group investigated a number of patient characteristics and found that only severity of illness was a predictor of residual symptoms., Conversely, for patients in full remission , Nierenberg and colleagues reported that the presence of residual symptoms was not predicted by baseline severity of depression. Some studies have found no relation between residual symptoms and life events., However, Opdyke et al reported that residual symptoms during continuation treatment in elderly patients who were in full remission were observed more often in subjects with associated severe life events or ongoing major stressors. Similarly, personality traits have been associated with residual symptoms in some studies but not in others.,
No relations have been found between residual symptoms and sociodemographic factors, family and personal history, follow-up care, comorbid conditions, chronic medical burden, social support or past or present illnesses.,, In addition, residual symptoms are prevalent, not only in patients who receive psychotherapy, but also in those treated with pharmacotherapy.
Hcc Coding: Major Depressive Disorder Specificity Makes A Difference
Imagine this scenario: today you saw one of your established patients, who is usually in a pleasant and talkative mood, but something was different. At first, they were quiet, only answering questions with a yes or no response and seemed to be avoiding any direct eye contact. They appeared tired and looked like they had lost weight. How do you determine HCC coding?
Once you started asking questions about their appearance, the patient starting crying and revealed that since the last visit 6 months ago, their spouse of 30 years was diagnosed with lung cancer and bone metastasis and was given a life expectancy of 3 months.
You May Like: How To Treat A Friend With Depression
Defining Depression And Its Impact On Self
In the DSM-5, major depressive disorder represents the classic condition in this group of disorders, unifying the other depressive disorders through the common characteristics of the presence of sad, empty or irritable mood, accompanied by somatic and cognitive changes that significantly affect the individuals capacity to function . The diagnostic language of the DSM-5 attempts to describe the experience of depression in words that are accessible to mental health professionals through standardization of language however, the words feel too far removed and flat to describe the reality of the psychological phenomenon . Unlike disease states of the physical body, the presence of major depressive disorder lacks easily observable and definitive biological markers and is therefore difficult to consistently assess through physical symptoms. Diagnosis in mental health thus remains an art as well as a science. Currently, the means of detecting depression are limited to subtle molecular and neural changes that are complicated to read and not yet unanimously endorsed .The path of major depressive disorder is often tracked through oral and written accountsthe development of the illness is relegated to the malleable world of words. Language serves as a signifier of experience, but is not always fully capable of explaining that experience.
Verbal Memory Functioning In Recurrent Depression During Partial Remission And Remission
- 1Department of Biological and Medical Psychology, University of Bergen, Bergen, Norway
- 2Division of Psychiatry, Haukeland University Hospital, University of Bergen, Bergen, Norway
- 3Moodnet Research Group, Haukeland University Hospital, University of Bergen, Bergen, Norway
The aim of the present study was to investigate verbal memory performance in a group of patients with remitted and partial remitted major depressive disorder. Thirty-one patients and 31 healthy matched controls were included in the study. Results from the California Verbal Learning Test show intact verbal memory performance in the patient group regarding learning, recall and recognition. However, patients had significantly poorer performance compared to healthy controls in immediate recall of the first trial in the verbal memory test. In conclusion, the patient group showed intact memory performance, when material is presented more than once. These findings indicate that memory performance in MDD patients with partial remission and remission benefit from repetition of material.
Also Check: Free Online Support Groups For Depression
How Is Response Defined When Is It Inadequate
Definitions related to antidepressant response matter because they affect treatment decisions. Nonresponse is often defined as less than 25% improvement on a standardized rating scale, and partial response, as more than 25% but less than 50% improvement.10 At least 50% reduction in symptomatology would indicate response,10 and remission would be defined as a cutoff score on a rating scale, such as 7 on the Hamilton Depression Rating Scale or < 5 on the PHQ-9, for at least 2 consecutive weeks.3,4
Remission is the treatment goal in MDD because it is associated with significant improvement in functioning as well as structural and metabolic changes that are not seen with only response.5,6 Failure to achieve remission typically results in residual symptoms, which are associated with increased risk of relapse, poorer outcomes, and decreased functioning.7
Nature Of Residual Symptoms
In a study of patients who remained partial responders to antidepressant therapy , 47% reported depressed mood, impairment of work and activities, psychic anxiety or sexual dysfunction, to at least a moderate degree. Symptoms that are more commonly associated with severe depression, including late insomnia, retardation, agitation, hypochondriasis, weight loss and loss of insight were less common. The most persistent residual symptoms reported in a study of elderly patients during the continuation phase of treatment were apathy, anxiety , anergia, insomnia, feelings of guilt and loss of libido. Although sexual dysfunction was reported in some studies surveyed, drug side effects were not systematically excluded from residual symptom scores.,
The 3 most common residual symptoms reported in a study of patients in full remission were sleep disturbances , fatigue and diminished interest or pleasure . Depressed mood and suicidal ideation were rarely reported. In another study of patients in full remission, the most common residual symptoms were generalized and somatic anxiety and irritability. When patients in remission were compared with a group of volunteers who had never been depressed, they demonstrated significantly more problems with social function, problem solving and dysfunctional attitudes.
Don’t Miss: Medication For Depression And Anxiety And Weight Loss
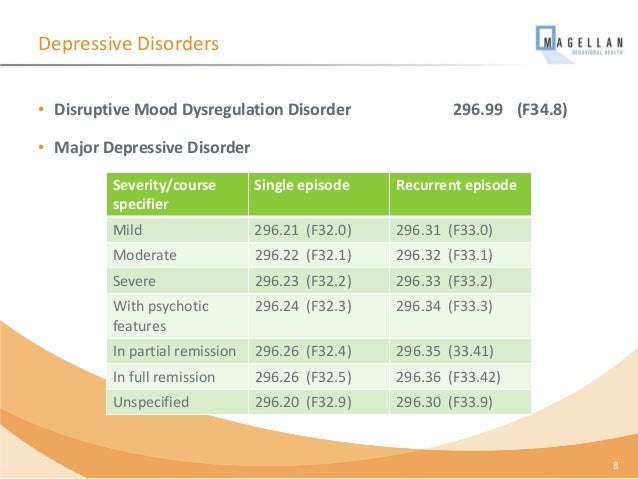
Criteria For Severity/psychotic/remission Specifiers For Current Major Depressive Episode
Note: These criteria are coded for in fifth digit of the DSM-IV diagnostic code. Can be applied to the most recent Major Depressive Episode in Major Depressive Disorder and to a Major Depressive Episode in Bipolar I or II Disorder only if it is the most recent type of mood episode.
.x1Mild: Few, if any, symptoms in excess of those required to make the diagnosis and symptoms result in only minor impairment in occupational functioning or in usual social activities or relationships with others.
.x2Moderate: Symptoms or functional impairment between mild and severe.
.x3Severe Without Psychotic Features: Several symptoms in excess of those required to make the diagnosis, and symptoms markedly interfere with occupational functioning or with usual social activities or relationships with others.
.x4Severe With Psychotic Features: Delusions or hallucinations. If possible, specify whether the psychotic features are mood-congruent or mood-incongruent:
.x5In Partial Remission: Symptoms of a Major Depressive Episode are present but full criteria are not met, or there is a period without any significant symptoms of a Major Depressive Episode lasting less than 2 months following the end of the Major Depressive Episode.
.x6In Full Remission: During the past 2 months, no significant signs or symptoms of the disturbance were present.
.x0Unspecified.
Last medically reviewed on May 17, 2016
The Nature And Treatment Of Residual Symptoms
What can be concluded regarding the nature of residual symptoms? There are various possibilities. Residual symptoms might represent persistent illness -the original illness continuing in milder form. Alternatively, they might, represent the phenomena preceding and underlying the depressive episode. Two possible aspects of the latter can substantially be discounted: subjects with residual symptoms are neither liable to be diagnosed as dysthymic nor, except to a minor degree, to show more personality abnormality than those who remit, fully. A third possible underlying phenomenon is that the residual symptoms could reflect, the cognitive vulnerability of dysfunctional attitudes. However, the symptoms shown by residual dépressives, although they include negative cognitions, are not limited to these, but include core mood and functional symptoms of depression. These are too wide to be related easily to a single abnormality of low self-esteem.
Recommended Reading: I Am Fat And Depressed
Three Phases Of Treatment Of Major Depression
Treatment consists of three phases:
Remission and relapse have been defined by the American Psychiatric Association. Remission is the return to the patients baseline level of symptom severity and functioning. Remission should not be confused with significant but incomplete improvement. Relapse is the re-emergence of significant depressive symptoms or dysfunction after remission has been achieved.
Acute Phase Treatment: Mild To Moderate
The combination of antidepressant medication and psychotherapy may be the initial treatment approach for patients with moderate depression in the presence of psychosocial stressors, interpersonal difficulties, intra-psychic conflict, and personality disorders. Combination therapy may also be appropriate for patients with only partial remission on one type of treatment, or with a history of poor adherence to treatment. Most primary care physicians can medically manage these patients while referring them to a professional psychotherapist for co-management.
Assessing for Adequate Response in the Acute Phase
Overall, if after the initial 4 8 weeks there is not a moderate improvement in baseline symptoms in the acute phase, then a reassessment of the diagnosis, medication regimen and / or psychotherapy, adherence, substance or alcohol use is in order. Increasing the treatment dose is the first step to be considered. If 4 8 weeks after the increase of treatment dose there is not a moderate improvement in symptoms, another review should occur. Other treatment options should then be considered in consultation with a psychiatric specialist.
You May Like: Is Ritalin Used For Depression
Implication For Practice: Cognitive Therapy Narrative Therapy Mood Memoirs And Empowering Metaphors
The DSM-5s medical model aligns with modernist approaches, which prioritize objectivity and tend to be more diagnostic in nature, often sustaining a power dynamic with therapist as expert and client as a subject therefore, when a clinician applies a particular diagnosis to an individual, he or she utilizes a rhetorical currency that only privileged professionals can speak with authority, excluding others from the conversation. The resulting power dynamic directly contradicts the National Association of Social Workers Code of Ethics, which emphasizes the importance of egalitarian partnership between professional and nonprofessional as critical for change . Cognitive therapy, narrative therapy, mood memoir writing, and engagement with metaphor are methods for changing the paradigm of depression from one of victimization to one of vanquishment.
Major Depressive Disorder Recurrent In Remission Unspecified
- 2016201720182019202020212022Billable/Specific Code
- F33.40 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
- Short description: Major depressive disorder, recurrent, in remission, unsp
- The 2022 edition of ICD-10-CM F33.40 became effective on October 1, 2021.
- This is the American ICD-10-CM version of F33.40 – other international versions of ICD-10 F33.40 may differ.
- Applicable To annotations, or
Also Check: Can Depression Make You Feel Emotionally Numb
The Key For Major Depression Disorder Recurrent Unveiled In 7 Basic Steps
Treatment aims to stop regressions of high or low episodes and also make the most of a persons lifestyle and also ability to work. A physician might additionally detect bipolar I condition if a persons past habits includes symptoms that fulfill the standards, or to put it simply, if a person has formerly had an episode that satisfies the criteria. The signs and symptoms of both depression as well as mania have to suggest a shift in the individuals actions or mood. There should additionally be no other major depression disorder recurrent factors that can explain the severe modifications in mood, such as substance abuse or a hormone imbalance. Bipolar depression may be more likely if an individual has one more mental health problem, such as obsessive-compulsive condition or traits of borderline individuality problem. Report any worries about negative effects to a healthcare service provider as soon as possible. The healthcare service provider may require to alter the dose or attempt a various medication.
What Are The Risk Factors For Recurrent Episodes And Treatment Resistance In Major Depressive Disorder
Twenty percent of individuals with major depressive disorder untreated at 1 year will continue to meet criteria for the diagnosis, whereas an additional 40% will have a partial remission. Pretreatment irritability and psychotic symptoms may be associated with poorer outcomes. Partial remission and/or a history of prior chronic major depressive episodes are risk factors for recurrent episodes and treatment resistance.
Also Check: How To Deal With A Depressed Spouse
Send Article To Kindle
To send this article to your Kindle, first ensure no-reply@cambridge.org is added to your Approved Personal Document E-mail List under your Personal Document Settings on the Manage Your Content and Devices page of your Amazon account. Then enter the name part of your Kindle email address below. Find out more about sending to your Kindle.Find out more about sending to your Kindle.