How To Treat And Prevent Depression Naturally
Since individuals with depression are seen to face a steeper cognitive decline in later years, it is advantageous to treat depressive symptoms right away. The longer your brain is exposed to the chemicals changes and stress associated with depression, the more cognition will fade.
Outside of therapy and medications for major depressive disorders, there are things you can do to fight feelings of depression. Improving your mood will be the best way to keep your brain young.
How The Brain Changes During Depression Treatment
- Date:
- University of British Columbia
- Summary:
- Researchers have shown what happens to the brain when a person receives a depression treatment known as repetitive transcranial magnetic stimulation . rTMS is a depression treatment typically used when other approaches — such as medications — haven’t been effective for a patient. By stimulating the dorsolateral pre-frontal cortex, rTMS activates several other regions of the brain involved in multiple functions, from managing emotional responses to memory and motor control.
For the first time, researchers have shown what happens to the brain when a person receives a depression treatment known as repetitive transcranial magnetic stimulation . The results were published today in the American Journal of Psychiatry.
rTMS is a depression treatment typically used when other approaches — such as medications — haven’t been effective for a patient. It is estimated that approximately 40 per cent of people with major depression do not respond to antidepressants.
During an rTMS session, a device containing an electromagnetic coil is placed against a patient’s scalp. The device then painlessly delivers a magnetic pulse that stimulates nerve cells in a region of the brain involved in mood control — called the dorsolateral pre-frontal cortex.
Although proven to be effective, the mechanisms behind how rTMS affects the brain have not been well understood.
Story Source:
Sleep Disturbances And Emotional Issues
The cortisol influx caused by depression can cause your amygdala to enlarge, increasing its activity. Since it helps control your emotions, damage to your amygdala can throw your emotions off balance. You may experience uncontrollable mood fluctuations as a result, causing you to experience both negative and positive emotions very intensely.
An enlarged amygdala doesnt just impede your emotional health and your mood stability its increased activity can also cause other issues, like sleep issues and disturbances. Sleep deprivation, in turn, can worsen your overreactions to stimuli. Poor sleep also causes you to develop a more negative mood and mindset, which can cause your depression to worsen.
Since this creates a feedback loop, issues with your amygdala can be one of the most dangerous things about major depressive disorder.
You May Like: Can You Get Disability For Bipolar Depression
Effects Of Depression On The Brain
Loss of serotonin and dopamines takes place at different rates among the depressed individuals. This would result in the variation in the nature, pattern, and severity of the symptoms of the brain during the depression.
- Serotonin Responsible for inhibiting pain and in the regulation of sleep, appetite, and mood. There is a connection between serotonin and depression in the sense that low levels of serotonin lead to higher risks for suicide.
- Dopamine Responsible for motivation, movement, and perception of reality. Any problem in the transmission of dopamine in the brain in its transmission would probably result in depression associated with psychosis and/or substance abuse.
- Norepinephrine This norepinephrine hormone helps in recognizing and responding to the stressful events and situations of life. Those with depression, may not have proper release and transmission of the neurotransmitter. This would result in an inability to handle stress effectively.
New Research Maps How The Brain Changes During Depression Treatment
Dr. Fidel Vila-Rodriguez performs rTMS on a study participant.
For the first time, researchers have shown what happens to the brain when a person receives a depression treatment known has repetitive transcranial magnetic stimulation . The results were .
Study participants received a round of rTMS within an MRI, allowing researchers to observe changes in the brain.
rTMS is a depression treatment typically used when other approaches such as medications havent been effective for a patient. It is estimated that approximately 40 per cent of people with major depression do not respond to antidepressants.
During an rTMS session, a device containing an electromagnetic coil is placed against a patients scalp. The device then painlessly delivers a magnetic pulse that stimulates nerve cells in a region of the brain involved in mood control called the dorsolateral pre-frontal cortex.
Although proven to be effective, the mechanisms behind how rTMS affects the brain have not been well understood.
When we first started this research, the question we were asking was very simple: we wanted to know what happens to the brain when rTMS treatment is being delivered, says Dr. Fidel Vila-Rodriguez, an assistant professor in UBCs department of psychiatry and researcher at the Djavad Mowafaghian Centre for Brain Health .
We wanted to know what happens to the brain when rTMS treatment is being delivered.Dr. Fidel Vila-Rodriguez
Don’t Miss: Residential Treatment Programs For Teenage Depression
A New Study Maps How The Brain Changes Throughout Depression Treatment
Researchers have for the first time shown what occurs in the brain during repetitive transcranial magnetic stimulation , a treatment for depression. On May 18, 2022, the findings were published in the American Journal of Psychiatry.
When other strategies, such as medications, have failed to help a patient with their depression, rTMS is often used as a treatment. Antidepressants are thought to be ineffective for around 40% of those who have serious depression.
A device with an electromagnetic coil is pressed on the patients scalp during an rTMS session. A painless magnetic pulse is then delivered by the device, stimulating nerve cells in the dorsolateral prefrontal cortex, a part of the brain involved in mood regulation.
Although rTMS has been shown to be effective, the mechanisms behind its effects on the brain are still poorly understood.
When we first started this research, the question we were asking was very simple: we wanted to know what happens to the brain when rTMS treatment is being delivered, says Dr. Fidel Vila-Rodriguez, an assistant professor at the University of British Columbias department of psychiatry and researcher at the Djavad Mowafaghian Centre for Brain Health .
To answer this question, Dr. Vila-Rodriguez and his team delivered one round of rTMS to patients while they were inside a magnetic resonance imaging scanner. Since the MRI can measure brain activity, the researchers were able to see in real-time what changes were happening in the brain.
Be Mindful Of Your Influences
Theres no shame in being protective over your morning routine.
Try to avoid things that can worsen your mood first thing in the morning, like frightening news stories or the endless social media scroll of people who you may be likely to compare yourself to.
Also, 2020 research shows that gratitude-based interventions may improve symptoms of depression and anxiety. You may find it useful to make a gratitude list first thing in the morning to help start your day.
You May Like: Lack Of Sleep Causes Depression
Residential Treatment Provides A Space To Heal
One of the most important reasons to choose residential care for depression treatment is that it gives you the space, the time, and the opportunity to truly focus on healing. There are no distractions of home, work, and other responsibilities, only a safe place to get better. The damage that depression has done to your brain and body can be slowed, stopped, and even reversed with good care.
The most effective treatment for depression is a combination of therapy and medications, both of which take time to work. This is another reason that residential treatment is a smart choice for depression care. It gives you time to develop a rapport with a therapist and to make positive changes. It also gives you a chance to try one or more antidepressants to find the medication that will adjust your brain chemicals in just the right way for maximum impact with fewest side effects.
Getting relief from depression through treatment will immediately begin to help your brain, reversing the shrinking of certain areas, the inflammation, and the overflow of cortisol. This in turn will help you feel better overall, and you will begin to get relief for the physical symptoms.
Bridges to Recovery offers comprehensive treatment for people struggling with mental health disorders as well as co-occurring substance use disorders. Contact us to learn more about our renowned Los Angeles-based program and how we can help you or your loved one start on the path to lasting wellness.
How Depression Changes Your Brain
It seems that more people in the world live with depression than ever before. In fact, according to the World Health Organization, an estimated 350 million people of all ages worldwide suffer from this mentally debilitating disease.
Depression can literally change your brain, altering the neural pathways and synapses and shrinking the size of your hippocampus, an area of the brain that regulates emotions and memory. Mentally, you probably feel foggy and exhausted, as your brain must work harder to process information and feelings. If you dont feel well mentally, it can take a toll on every other area of your life.
Depression can make you feel disconnected from the world around you, helpless to make any sort of change, and paralyzed by the thoughts inside your head. To combat all of these feelings, many people unfortunately turn to prescription drugs as a temporary answer, but we still dont know the long-term effects of these powerful drugs. Instead of medicating ourselves, we can turn to more natural remedies that often work better than even pills can.
Today, well go over how exactly depression alters your brain, and ways to reverse the damage naturally. It takes willpower and determination, but you CAN take your life back with a few simple lifestyle changes and ways of thinking.
You May Like: Does Lack Of Sunlight Cause Depression
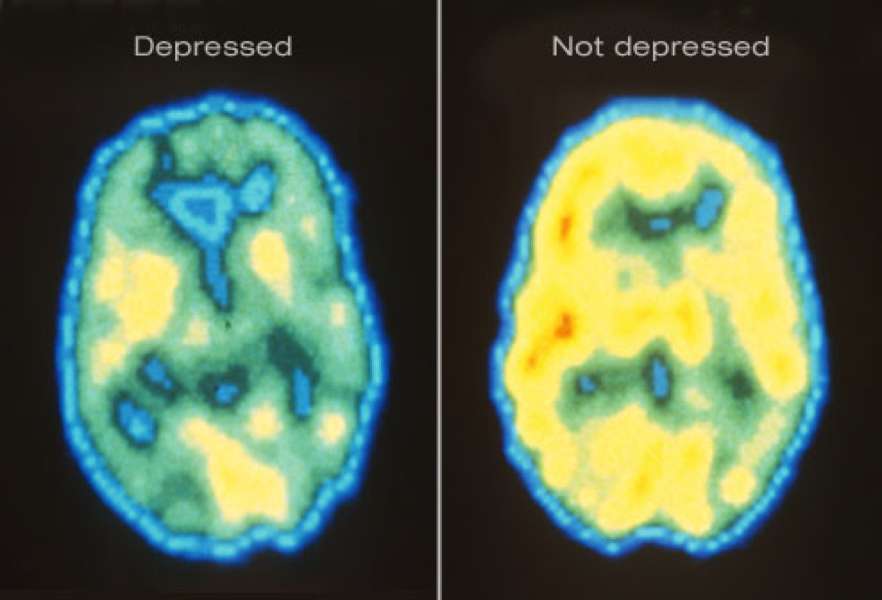
Regions That Affect Mood
Increasingly sophisticated forms of brain imaging such as positron emission tomography , single-photon emission computed tomography , and functional magnetic resonance imaging permit a much closer look at the working brain than was possible in the past. An fMRI scan, for example, can track changes that take place when a region of the brain responds during various tasks. A PET or SPECT scan can map the brain by measuring the distribution and density of neurotransmitter receptors in certain areas.
Use of this technology has led to a better understanding of which brain regions regulate mood and how other functions, such as memory, may be affected by depression. Areas that play a significant role in depression are the amygdala, the thalamus, and the hippocampus .
Research shows that the hippocampus is smaller in some depressed people. For example, in one fMRI study published in The Journal of Neuroscience, investigators studied 24 women who had a history of depression. On average, the hippocampus was 9% to 13% smaller in depressed women compared with those who were not depressed. The more bouts of depression a woman had, the smaller the hippocampus. Stress, which plays a role in depression, may be a key factor here, since experts believe stress can suppress the production of new neurons in the hippocampus.
Your Brain Needs More Energy: Glucose
When youre suffering from depression, your brain is incredibly active. It may seem strange, but scientific studies say that a depressed brain activates many parts of the brain.
Why?
Its easy to understand. When youre depressed, you remember, think, suffer and reason in search of solutions and new alternatives. Its also harder to sleep because youre thinking about so many different things. Your hippocampus is therefore active, which is the front part of the brain . In addition, the anterior cingulate cortex and the temporal lobes are more active.
You also have to keep in mind that your brain uses almost 20% of your energy.
However, when youre depressed, it needs even more, with glucose being the main need. This causes you to feel more hungry and to seek sweet things, for example. Sometimes, this is the reason why many gain weight when theyre sad or depressed.
You May Like: Latuda For Bipolar 2 Depression
Whats Happening In The Brain In Major Depressive Disorder
Many different combinations of symptoms lead to a diagnosis of depression, and the many different subtypes and symptoms of depression are produced by molecular, cellular, and network interactions in the brain. An overview of current understanding of these interactions was presented at ECNP 2021 by Professor Gitte Moos Knudsen, Copenhagen, Denmark.
Changes in the brain linked to major depressive disorder
Major depressive disorder is a heterogeneous disease with many combinations of symptoms
Although major depressive disorder is often thought about as one disease, it is clear there are many subtypes, said Professor Knudsen, who highlighted current understanding of the variety of biological mechanisms linked to MDD, including:
- Altered neurotransmission involving the monoamines and the glutaminergic and GABAergic systems. The monoamine theory for MDD based on a lack of serotonin and to some extent noradrenaline has prevailed many years, said Professor Knudsen, but now the glutamatergic and GABAergic systems are also considered to play an important role.1
Altered neurotransmission in major depressive disorder involves the monoaminergic, glutamatergic, and GABAergic systems
The default mode network plays a role in major depressive disorder
Anatomic changes in the brain in MDD include:
Hippocampal atrophy is a notable anatomic change in major depressive disorder
Impaired adaptive signaling results in the core symptoms of major depressive disorder
Brain Chemicals And Depression
Researchers have suggested that for some people, having too little of certain substances in the brain could contribute to depression. Restoring the balance of brain chemicals could help alleviate symptomswhich is where the different classes of antidepressant medications may come in.
Even with the help of medications that balance specific neurotransmitters in the brain, depression is a highly complex condition to treat. What proves to be an effective treatment for one person with depression may not work for someone else. Even something that has worked well for someone in the past may become less effective over time, or even stop working, for reasons researchers are still trying to understand.
Researchers continue to try to understand the mechanisms of depression, including brain chemicals, in hopes of finding explanations for these complexities and developing more effective treatments. Depression is a multi-faceted condition, but having an awareness of brain chemistry can be useful for medical and mental health professionals, researchers, and many people who have depression.
Depression Discussion Guide
Also Check: Methods Of Therapy For Depression
What Happens In The Brain During A Major Depressive Episode
At any one time, 4% of the population is experiencing a major depressive episode,1 said Professor Jeffrey Meyer, University of Toronto, Canada, at WCP 2021 and 50% of MDD episodes do not respond to treatment.2 New imaging techniques show differences in the regions of the brain and neural circuits involved in major depressive disorder between patients who do and patients who do not respond to treatment.
Evidence for microglial activation and neuroinflammation
Microglia are activated during a major depressive episode
Microglial activation plays a key role in neuroinflammation and is implicated in neuroprogression, said Professor Meyer. It can be demonstrated by measuring translocator protein , which is a marker for microglial activation.3
The total distribution volume of translocator protein is measured using positron emission tomography 3 and studies demonstrate consistently increased TSPO VT and therefore microglial activation in major depressive disorder .4
Professor Meyer highlighted that the increase in TSPO VT in patients during a major depressive episode is greater in those who have had:
- A longer duration of illness3
- Long periods of no antidepressant treatment3
Microglial activation occurs in regions of the brain implicated in MDD
Microglial activation involves the neural circuits implicated in MDD
The TSPO VT distribution therefore involves the neural circuits that have been implicated in MDD,4 he explained.
How Does Clinical Depression Affect The Brain
Even though clinical depression largely affects how an individual feels, depression is more than feeling sad. Most people feel sad from time to time. Individuals who are clinically depressed experience prolonged periods of hopelessness. One of the primary distinctions between temporarily feeling down and clinical depression is the effect each experience has on the brain.
Individuals dealing with the normal ups and downs of life may cry, feel upset, and avoid friends and family for temporary periods of time. They might even sleep in or stay up all night. But ultimately, their ability to function, complete tasks, and maintain responsibilities remains the same. They bounce back from their sadness and their brain, for the most part, remains mostly unaffected.
Individuals living with clinical depression, however, dont recover from their feelings of hopelessness and sadness as easily. Their symptoms can linger for weeks, months, or years. They struggle to function like they once did. Even managing small tasks and responsibilities can become difficult. This is because clinical depression can physically change the brain, the bodys command center.
Research shows that clinical depression can in fact:
- Shrink the brain
- Reduce oxygen levels in the brain
You May Like: Cognitive Behavioral Therapy For Depression And Anxiety
Onset Of Depression More Complex Than A Brain Chemical Imbalance
It’s often said that depression results from a chemical imbalance, but that figure of speech doesn’t capture how complex the disease is. Research suggests that depression doesn’t spring from simply having too much or too little of certain brain chemicals. Rather, there are many possible causes of depression, including faulty mood regulation by the brain, genetic vulnerability, stressful life events, medications, and medical problems. It’s believed that several of these forces interact to bring on depression.
To be sure, chemicals are involved in this process, but it is not a simple matter of one chemical being too low and another too high. Rather, many chemicals are involved, working both inside and outside nerve cells. There are millions, even billions, of chemical reactions that make up the dynamic system that is responsible for your mood, perceptions, and how you experience life.
With this level of complexity, you can see how two people might have similar symptoms of depression, but the problem on the inside, and therefore what treatments will work best, may be entirely different.
What follows is an overview of the current understanding of the major factors believed to play a role in the causes of depression.