What Causes Cognitive Impairment
Cognitive impairment is not created by a single disease or a single There are, however, several conditions, resulting from changes in the brain, that may cause cognitive impairment. For example:
- Dementia like Alzheimers disease
- Traumatic brain injury
- Lewy bodies clumps of protein in the brain
- Reduction or enlargement of certain areas of the brain
Two symptoms that people experience, if cognitively impaired, are forgetfulness and confusion. In the same way, there are conditions that may bring about similar symptoms:
- Sleep disorders
- Illness
Practical Treatment Approaches Based On Available Evidence
Dr Culpepper summed up his discussion by stating that after evaluating the available evidence, depression can be seen as a disorder that involves a complex set of changes, many of which impact cognition, and these, in turn, may affect symptom severity and functional impairment. Insights into available treatment modalities have demonstrated their effects on the neural basis of cognition. On the basis of these insights, the treatment of cognitive impairment in depression should focus on effectively alleviating mood symptoms. For many patients, this will lead to improvement in cognition. For patients with significant cognitive impairment at baseline, treatment with an agent that has demonstrated efficacy, and particularly those that have direct efficacy, in cognition may be warranted, or augmentation with an adjunctive pharmacologic agent such as a psychostimulant or cognitive enhancer may be considered, or a psychological intervention may be added.
Does Depression Cause Cognitive Dysfunction
Issues with depression and cognitive dysfunction have been acknowledged for a long time but previously, it was often thought to be secondary to the other symptoms of depression. For example, due to lack of motivation , it was thought that people with depression simply weren’t motivated to accomplish the cognitive tasks asked of them.
Now, however, researchers believe this not to be true. Not only do we know of the cognitive deficits present during acute depressive episodes but we also know that some cognitive deficits do not completely go away even when depression is in remission. Impairments in memory are one such deficit that has been shown to be present even when the person is in recovery, independent of medication status.Additionally, through brain scans, it is now known that depression negatively affects brain volume in some areas and that may be one reason people experience impaired functioning in cognitive areas.
Read Also: How To Help Your Husband With Depression
Other Causes Of Cognitive Dysfunction In Depression
Of course, it’s also important to remember that improper dosing of depression medication can also cause cognitive impairment in depression. If someone is taking too high a dose of an antidepressant or antipsychotic, for example, they may exhibit similar, or worsening, symptoms of cognitive deficits. Careful work with a doctor can prevent this from occurring.
Drug and alcohol abuse can also cause, or worsen, cognitive deficits and this, unfortunately, is all too common in people with major depressive disorder.
Finally, cognitive deficits also appear to be more pronounced the more an individual with depression focuses on their depression . This is often seen when people are under greater than usual amounts of stress.
What Is Major Depressive Disorder
Major depressive disorder, or simply depression, is a common, treatable, mental health problem. You may feel sad and lose interest in activities you once enjoyed. It can lead to problems in your work and home life as well as other emotional and even physical problems. It could also cause:
- Pacing, handwringing, and other restless activities
- Slowed speech and movements that others notice
- Difficulty focusing on tasks or making decisions
- Changes in appetite
- Remember or think of information
- Process or “make sense of” new information quickly
- Respond to new information in an appropriate way
If you lose some of these abilities, your quality of life may not be as good as it once was. You may not be able to function at work. You also might not respond as well to your treatment and could face a higher risk of another bout with depression.
Some evidence suggests that your thinking skills, once they start to decline from depression, could continue to worsen, even at times when you don’t feel especially depressed.
Don’t Miss: How To Get Up When Depressed
Where Do You Get Cognitive Remediation For Depression
Your primary care doctor can help connect you with a mental health specialist who treats depression. Different therapists use different approaches, sometimes including cognitive remediation.
Before you schedule an appointment, you can ask a therapist whether they use cognitive remediation and whether they would consider the treatment for your particular case.
If you already have a therapist that you see regularly, ask them whether cognitive remediation could be an appropriate tool for you.
Another option is to go to a group cognitive remediation session. You may need a referral to attend some of these groups. A mental health professional familiar with cognitive remediation would be the best guide for group treatment.
Show Sources
Other Causes Of Memory Loss
Other reasons you may experience memory loss can include the following:
- Normal age-related memory loss is common and manageable. One example of this is forgetting where you put your glasses but remembering later in the day.
- Alzheimers disease is the most common form of dementia. It can cause progressive, irreparable brain damage and memory loss.
- Mild cognitive impairment can alter thinking skills and eventually progress to Alzheimers disease or other forms of dementia.
- Minor head injury or trauma can trigger slight memory problems, even if you didnt lose consciousness.
- Forgetfulness is a potential side effect of certain medications.
- Brain tumors or brain infections can affect your memory or trigger dementia-like symptoms.
- Vitamin B-12 deficiency can create problems with your memory. This is because youre not maintaining healthy nerve cells and red blood cells.
- Alcoholism or drug abuse can impair your mental state and abilities. This can also occur when alcohol interacts with medications.
- Hypothyroidism slows your metabolism, which can lead to memory problems and other issues with thinking.
- Brain or nerve damage caused by diseases such as Parkinsons disease or multiple sclerosis can cause memory problems. A 2013 study found that people with depression have a greater risk of developing Parkinsons disease.
Recommended Reading: Is Major Depression A Mood Disorder
Psychiatric Conditions Contribute To Cognitive Impariment
Since theyre mental illnesses, its little surprise that cognitive impairment can result from psychiatric conditions. They also connect to late-life psychosis, paranoia, thinking issues, memory problems, and lack of concentration.
While the symptoms of most psychiatric conditions involve some degree of cognitive deficit, cognitive impairment is most common in disorders such as:
· Schizophrenia
Studies prove that schizophrenia can present with multiple different types of cognitive impairment. This disorder has no prominent neuropsychological signature, so exact impairments exist across patients in various styles and severities. Common issues involve working memory, attention, general intelligence, verbal learning, verbal fluency, and executive function.
· Bipolar Disorder
The exact details of cognitive impairment among those with bipolar disorder arent very well-understood. Still, research has shown that many patients with the condition experience various neuropsychological struggles. These struggles mainly involve long-term memory, attention, declarative function, and executive function.
· Major Depressive Disorder
· Anxiety Disorders
More Than Sad: Depression Affects Your Ability To Think
- By James Cartreine, PhD, Contributing Editor
ARCHIVED CONTENT: As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date each article was posted or last reviewed. No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.
When you think of clinical depression, you probably think of feeling sad and down for long periods of time losing your energy and your interest in things you used to enjoy sleeping too much or too little, or eating too much or too little. But besides these, depression can actually change your ability to think. It can impair your attention and memory, as well as your information processing and decision-making skills. It can also lower your cognitive flexibility and executive functioning .
For people with severe depression, medications can provide some relief of low mood and energy, bolster the motivation to engage in enjoyable and important activities, and help people return to normal sleeping and eating patterns.
But we dont know whether antidepressant medications treat cognitive impairment related to depression. Recently, an international research team attempted to answer this question as part of a larger study on depression treatment. Their results were published in The Lancet last month.
Read Also: How To Control Depression Thoughts
Assessment Of Cognitive Dysfunction In Major Depressive Disorder
The bias toward negative cognitive schemes found in MDD is likely to contribute, at least in part, to the high percentage of patients reporting subjective cognitive complaints during depressive episodes. The discordance between subjective complaints and objective measures of cognitive dysfunction highlights the importance of clinically based screening for both subjective and objective cognitive functioning. However, one of the key clinical challenges is in the lack of consensus on best tools to accurately and efficiently assess cognition in clinical settings. No single test or test battery has emerged as the gold standard in MDD. This is in contrast to initiatives, such as the Measurement and Treatment to Improve Cognition in Schizophrenia Consensus Cognitive Battery, developed to evaluate the impact of new medications on cognition in schizophrenia,26 and a similar consensus battery to assess neurocognition in BD.27
Regardless of the distinction between subjective and objective findings of cognitive impairment during an MDE,18 subjective cognitive complaints should trigger additional investigation into sleep quality and other medical comorbidities, as these factors are known to negatively affect cognitive performance.7 For example, sleep may have pro-cognitive effects28 and sleep deprivation affects numerous domains of cognition.29
Cognitive Distortions And Mental Health
Conditions such as depression and anxiety can sometimes lead to habitual negative thoughts, but in many cases, depression actually is the result of cognitive distortions.
When bad things happen, we begin chastising ourselves with thoughts such as I’m no good, I’m a total failure or Nothing ever goes my way. Our feelings follow what we are thinking, and negative thoughts like these can ultimately contribute to symptoms of depression.
This concept is the guiding principle behind cognitive therapy, a type of psychotherapy developed by psychiatrist Aaron T. Beck in the 1960s. If we think something often enough, we begin to believe it’s true and our feelings match what we are thinking about ourselves.
To manage depression, we must stop those automatic negative thoughts and replace them with more positive, truthful ones. By nipping these thoughts in the bud, we can sometimes halt depression before it even starts.
You May Like: Guided Meditation For Anxiety And Depression
Evaluation And Treatment Of Depression May Reverse Memory And Cognitive Difficulties In Older Adults With Mild Cognitive Impairment
Individuals with worse depression and mood symptoms are more likely to develop Mild Cognitive Impairment and to progress from MCI to dementia. Evaluation and treatment of symptoms of depression may improve or maintain cognitive functioning in some older patients diagnosed with MCI.
MCI is a state in between normal cognition and Alzheimers disease dementia, in which the individual has a subjective complaint of memory and other cognitive difficulties and performance on formal neuropsychological testing is abnormal for age, but these problems do not interfere with routine independent functioning. The majority of people with MCI have progressive memory and cognitive impairment, and eventually are unable to function independently with daily tasks, resulting in a diagnosis of dementia. However, some individuals with MCI do not get progressively worse and some people improve, reverting back from MCI to normal cognition. This study demonstrated that measuring neuropsychiatric symptoms such as depression, anxiety, agitation and irritability, helps to predict who will progress from normal cognition to MCI, and then who will either progress from MCI to AD dementia or revert back to normal cognition.
Depression As A Risk Factor

It is well established that depression is a risk factor for dementia, but speculation still exists that the cognitive dysfunction occurring with depression leads to the decline and impairment recognized as dementia. More research has been done to establish what type of depression predicts the development of dementia results show that early-onset or late-onset , are the most likely to lead to dementia later in life.
A study done in Nature Review Neurology affirmed the correlation between depressive symptoms early in life, and the magnified increase in dementia risk.
For older people already suffering from dementia, depression may manifest itself as physical symptoms, rather than its commonly known cognitive symptoms. These symptoms can include a loss of appetite or energy. This does not discount the many cognitive symptoms that can appear as a result of depression the Alzheimer’s Society provides a comprehensive list of these symptoms on their website.
Recommended Reading: What Do People Do When They Are Depressed
What Is Cognitive Remediation
Cognitive remediation is a treatment for some types of cognitive impairment. It gives you a set of tools to improve attention, memory, and other brain functions that can worsen with depression.
The aim is to improve your quality of life and productivity at work or school and in social situations. The strategies in cognitive remediation vary, but you might do some of the following exercises:
- Write in a notebook or daily planner to remind you of important tasks and deadlines
- Break tasks down into a logical set of steps to help you complete them
- Practice attention and thinking exercises to help improve your ability to hold onto and recall information
- Set goals with a health care provider to customize your treatment and track your progress
You can use these strategies on your own, but they tend to work even better with the help of a therapist or support group.
Cognitive Symptoms And Pharmacotherapy Of Depression
Independently of the severity of symptoms neurocognitive deficits predict worse therapeutic response during SSRI pharmacotherapy in young and elderly patients also after correcting for severity of depressive symptoms . However, interaction between cognitive impairment and pharmacotherapy is bidirectional more severe cognitive deficits indicate not only worse response to SSRI pharmacotherapy, but treatment in many cases negatively impacts cognitive functioning. In one study one quarter of SSI-treated patients reported loss of creativity, and other cognitive side effects including concentration difficulties, loss of ambition, memory and problem solving capacity impairment . Patients treated with newer antidepressants do better from a cognitive aspect compared to untreated patients, but still perform worse compared to healthy controls . As we emphasized, cognitive disturbances are among the most common residual symptoms of depression in spite of treatment, which reflects that currently available antidepressants are not able to sufficiently improve cognitive symptoms of depression.
Serotonergic dysfunction and cognitive symptoms of depression
Recommended Reading: How To Feel Less Depressed And Anxious
Variables Associated With Ci In Mdd
As described in the previous section, empirical evidence suggests that CI might be an important factor contributing to poorer functional outcome in MDD, and consequently may be referred to as clinically relevant. In consequence, the examination of variables associated with persisting CI in MDD might help to better understand underlying mechanisms as well as identify possible risk groups regarding the development of CI in the course of illness.
A number of variables associated with CI have been thoroughly analyzed and described in literature, for example, various demographic variables like age , educational attainment , and employment status . Also, variations concerning disease variables and psychopathology, like onset of disorder , duration of illness , number of past hospitalizations , and current symptom severity have been found to be associated with the development of CI and the degree to which it presents itself in MDD patients. Some of the inconsistencies in literature regarding the prevalence and profile of CI in depression might be due to complex interactions between these variables.
Depression And Cognitive Deficits
Cognitive deficits refer to the specific areas in which cognitive dysfunction is seen and depression is associated with five areas of cognitive deficits:
Not all studies show the same cognitive impairment levels or areas, but what does seem consistent throughout research studies is that:
- Not all people suffer from cognitive dysfunction in depression
- Not all people with depression experience cognitive dysfunction in the same ways
- More severe depressions produce greater cognitive dysfunction
- More incidences of depression cause greater cognitive dysfunction
- Older individuals with depression suffer from greater cognitive dysfunction
- Psychotic depression produces greater levels of cognitive dysfunction
Video courtesy of Global Medical Education
Don’t Miss: Who Do You See If You Have Depression
Cognitive Symptoms During Depression
ICD and DSM mention cognitive disturbances during depression only in general, most studies, however, describe a wide range of cognitive dysfunctions during the acute phase of depression. Research indicates that verbal and visual short and long-term memory, executive functions, psychomotor skills and attention are all impaired in depressed patients . Results, however, are somewhat contradictory, in part because studies investigate patients of different age with different clinical characteristics, illness course and medication schemes with differing methodology. Furthermore, several studies observed sustained cognitive deficits also in patients in remission . Patients in everyday clinical practice also report complaints reflecting cognitive dysfunctions, and clinicians do not necessarily associate part of these complaints with cognitive dysfunctions therefore, their recognition may be problematic .
Table 1 Symptoms reflecting cognitive dysfunctions reported by patients in everyday clinical practice
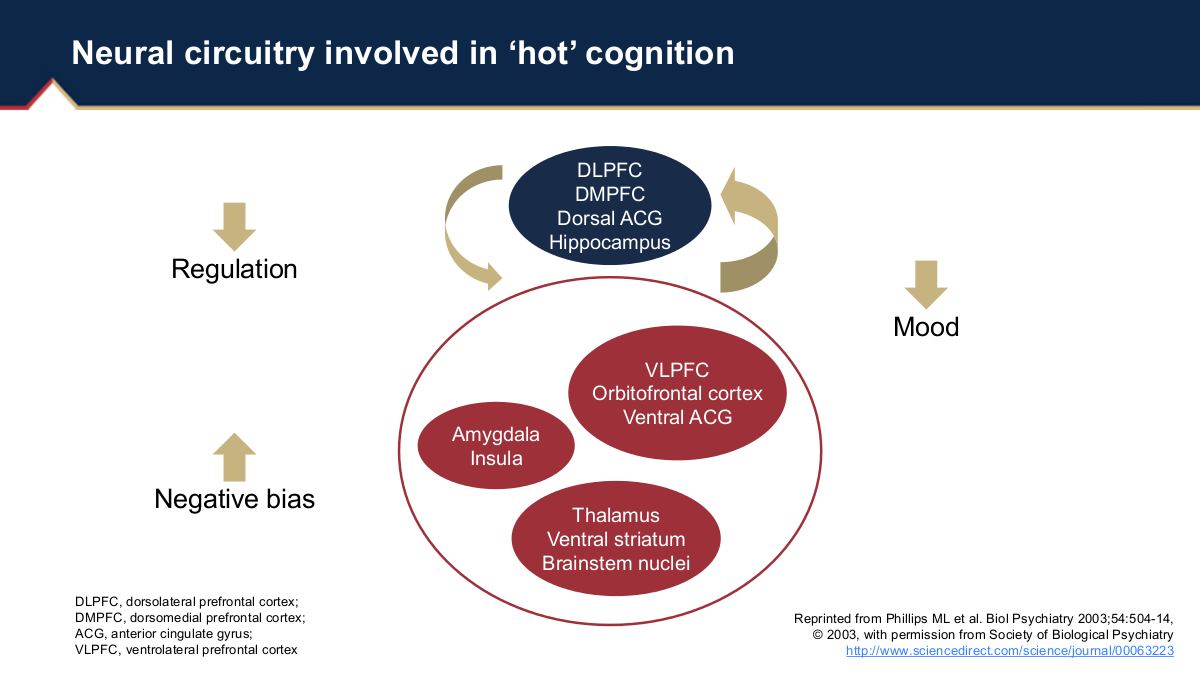
Hot and cold cognitive symptoms
Cognitive neuropsychological theory of depression
Trait- and state-like cognitive deficits during depression
Depression And Cognitive Dysfunction
Can Depression Cause Cognitive Impairment ?
Most people think of depression as causing emotional changes, but can depression cause cognitive impairment too? Studies show that not only does depression cause emotional and physical symptoms, but it also causes cognitive dysfunction . Cognitive dysfunction is also seen in bipolar disorder and quite markedly in schizophrenia. If you’re wondering, “Do I have cognitive dysfuction because of depression?”, take our Cognitive Symptoms of Depression Test. It’s free and instantly scored.
Don’t Miss: How To Cure Clinical Depression