Life Expectancy And The Risk Of Suicide
Depressed individuals have a shorter life expectancy than those without depression, in part because people who are depressed are at risk of dying of suicide. Up to 60% of people who die of suicide have a mood disorder such as major depression, and the risk is especially high if a person has a marked sense of hopelessness or has both depression and borderline personality disorder. About 2â8% of adults with major depression die by suicide, and about 50% of people who die by suicide had depression or another mood disorder. The lifetime risk of suicide associated with a diagnosis of major depression in the US is estimated at 3.4%, which averages two highly disparate figures of almost 7% for men and 1% for women . The estimate is substantially lower than a previously accepted figure of 15%, which had been derived from older studies of people who were hospitalized.
Depressed people have a higher rate of dying from other causes. There is a 1.5- to 2-fold increased risk of cardiovascular disease, independent of other known risk factors, and is itself linked directly or indirectly to risk factors such as smoking and obesity. People with major depression are less likely to follow medical recommendations for treating and preventing cardiovascular disorders, further increasing their risk of medical complications.Cardiologists may not recognize underlying depression that complicates a cardiovascular problem under their care.
Major Depressive Disorder Description And Dsm
Major Depressive Disorder description and DSM-5 codes
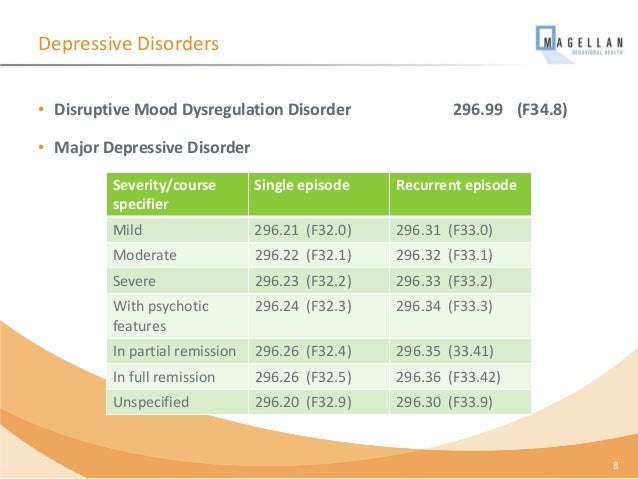
Major depressive disorder is a type of psychiatric illness in which the patients thoughts, moods, and behavior patterns are affected for a long period . The illness causes distress to the patient and affects his or her life socially, and eventually impairs his or her quality of life. A major depressive disorder is characterized by loss of interest in the activities the person once enjoyed, sadness, lack of sleep, change in body weight, and high suicidal thoughts. MDD is a DSM-5 diagnosis given the F32 code. Different levels of MDD are given other codes. MDD mild is given F32.0, moderate given F32.1, severe without psychotic features given F32.2, severe with psychotic features given F32.3, MDD in partial remission as F32.4 and MDD full remission given F32.5.
Psychological model
Major depressive disorder best fits in the cognitive-behavioral that describes that major depression results from distorted thinking and judgments. This cognitive behavior can be learned from the environment that we are in. For example, a dysfunctional family member may develop significant depression from stressful experiences or traumatic events. People with depression think differently from people who are not depressed, and the negative thoughts make the depression worse. Depression first manifests in negative thoughts before it causes adverse effects on the patient and their lives.
Etiology of major depression
Depression And The Covid
The Centers for Disease Control and Prevention conducted a survey Mental Health, Substance Use, and Suicidal Ideation During the COVID-19 Pandemic United States, June 2430, 2020 and reported that The coronavirus disease 2019 pandemic has been associated with mental health challenges related to the morbidity and mortality caused by the disease and to mitigation activities, including the impact of physical distancing and stay-at-home orders. Symptoms of anxiety disorder and depressive disorder increased considerably in the United States during AprilJune of 2020, compared with the same period in 2019. The full survey and results can be found on the CDC website .
A more recent article from April 6, 2021, in the AMAs publication Journal of the American Medical Association CDC Study Finds Worsening Anxiety and Depression, Especially in Young Adults, During COVID-19 Pandemic reports the findings of the online survey of 800,000 adults conducted from August 19, 2020 to February 1, 2021.
When you follow the link above, note the numerous additional articles that appear in the column to the right of the article itself.
These are just two references from reputable sources, the CDC and the AMA. We advise caution when using information from sources without first determining potential bias.
Don’t Miss: How To Notice Someone Is Depressed
F322 Severe Depressive Episode Without Psychotic Symptoms
In a severe depressive episode, the sufferer usually shows considerable distress or agitation, unless retardation is a marked feature.
Loss of self-esteem or feelings of uselessness or guilt are likely to be prominent, and suicide is a distinct danger in particularly severe cases. It is presumed here that the somatic syndrome will almost always be present in a severe depressive episode.
Major Depressive Disorder Single Episode Unspecifiedf329

Chapter 5 – Mental, Behavioral and Neurodevelopmental disorders » Mood disorders » Major depressive disorder, single episode, unspecified
Hierarchy Tree View
YOU AGREE THAT THE INFORMATION PROVIDED ON THIS WEBSITE IS PROVIDED AS IS, WITHOUT ANY WARRANTY OF ANY KIND, EXPRESSED OR IMPLIED, INCLUDING WITHOUT LIMITATION WARRANTIES OF MERCHANTABILITY OR FITNESS FOR ANY PARTICULAR PURPOSE, OR NON-INFRINGEMENT OF ANY THIRD-PARTY PATENT, COPYRIGHT, OR ANY OTHER THIRD-PARTY RIGHT. IN NO EVENT SHALL THE CREATORS OF THE WEBSITE OR WASHINGTON UNIVERSITY BE LIABLE FOR ANY DIRECT, INDIRECT, SPECIAL, OR CONSEQUENTIAL DAMAGES ARISING OUT OF OR IN ANY WAY CONNECTED WITH THE WEBSITE, THE USE OF THE WEBSITE, OR THIS AGREEMENT, WHETHER IN BREACH OF CONTRACT, TORT OR OTHERWISE, EVEN IF SUCH PARTY IS ADVISED OF THE POSSIBILITY OF SUCH DAMAGES.
Recommended Reading: How To Get Back From Depression
Can Major Depression Be Prevented
Once you have had an episode of major depression, you are at high risk of having another. The best way to prevent another episode of depression is to be aware of the triggers or causes of major depression and to continue taking the prescribed medication to avoid relapse. It is also important to know what the symptoms of major depression are and to talk with your doctor early if you have any of these symptoms.
Show Sources
Depression Nos Vs Major Depressive Disorder
Lets circle back to one of the main reasons for this revision. Recall that the DHCS stated that the default code for depression NOS was clinically incorrect, and having an unspecified term default to major depression will prevent the true incidence of depression NOS from being captured and will incorrectly increase the incidence of major depression in statistical data.
Essentially, without a default code for depression NOS,, patients diagnosed with unspecified depression are included in the data with patients or clients diagnosed with major depressive disorder. There is no way to distinguish one from the other if both are assigned code F32.9.
The American Psychiatric Association publication Diagnostic and Statistical Manual of Mental Disorders is the best and most comprehensive resource that explains the many diagnoses and criteria in detail. We are not permitted to reprint anything from the DSM-5 here, we can, however, provide simplified definitions of depression, unspecified, and major depressive disorder compiled from other sources. Recall that the APA reviewed and supported the code modifications.
Fun factoids
- The abbreviation NOS is not used in DSM-5.
- In ICD-11, the abbreviation NOS appears as part of inclusion terms under code 6A7Z Depressive disorders, unspecified. ICD-11 code 6A7Z includes the diagnoses depression, NOS, depressed, NOS, and depressive disorder, NOS.
Terms defined
You May Like: Valerian For Anxiety And Depression
What Is Major Or Clinical Depression
Most people feel sad or low at some point in their lives. But clinical depression is marked by a depressed mood most of the day, sometimes particularly in the morning, and a loss of interest in normal activities and relationships — symptoms that are present every day for at least 2 weeks. In addition, according to the DSM-5 — a manual used to diagnose mental health conditions — you may have other symptoms with major depression. Those symptoms might include:
- Fatigue or loss of energy almost every day
- Feelings of worthlessness or guilt almost every day
- Impaired concentration, indecisiveness
- Insomnia or hypersomnia almost every day
- Restlessness or feeling slowed down
- Recurring thoughts of death or suicide
- Significant weight loss or gain
Hcc Coding: Major Depressive Disorder Specificity Makes A Difference
Imagine this scenario: today you saw one of your established patients, who is usually in a pleasant and talkative mood, but something was different. At first, they were quiet, only answering questions with a yes or no response and seemed to be avoiding any direct eye contact. They appeared tired and looked like they had lost weight. How do you determine HCC coding?
Once you started asking questions about their appearance, the patient starting crying and revealed that since the last visit 6 months ago, their spouse of 30 years was diagnosed with lung cancer and bone metastasis and was given a life expectancy of 3 months.
Read Also: How Do You Know If You Are Suffering With Depression
What Is The Outlook For Someone With Major Depressive Disorder
While someone with MDD can feel hopeless at times, its important to remember that the disorder can be treated successfully. There is hope.
To improve your outlook, its critical to stick with your treatment plan. Dont miss therapy sessions or follow-up appointments with your healthcare professional.
Never stop taking your medications unless your therapist or healthcare professional advises you to.
On days when you feel particularly depressed despite treatment, it can be helpful to call a local crisis or mental health service or the National Suicide Prevention Lifeline. Resources are available.
A friendly, supportive voice could be just what you need to get you through a difficult time.
Major Depressive Disorder Single Episode Moderate
- 2016201720182019202020212022Billable/Specific Code
- F32.1 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
- The 2022 edition of ICD-10-CM F32.1 became effective on October 1, 2021.
- This is the American ICD-10-CM version of F32.1 – other international versions of ICD-10 F32.1 may differ.
- Applicable To annotations, or
Recommended Reading: What To Do When You Feel Depressed And Unmotivated
Most Commonly Used Icd
If youre wondering about trends in mental health over the past year, youre not the only one. To get more insight into the usage and trends of the behavioral health community in 2021, we identified the most common ICD-10 codes used by SimplePractice customers.
This data on the most frequently used ICD-10 codes is pulled from SimplePractice customers who have billed insurance over the last calendar year, so this report represents common diagnostic codes used by solo or small group providers in the behavioral health space across the country.
Valant Electronic Health Record Makes Entering Icd
Valant recently created a cheat sheet for all new ICD-10 codes replacing ICD-9 codes 296.32 to 331.0. Our reference also includes new codes for V58.69 and V71.09.
Clinicians using Valants intuitive EHR software can create, store, and organize diagnoses in the patients digital chart within our application. Valant EHR software supports clients transitioning from ICD-9 to ICD-10 codes by automatically updating to the latest code version. We invite mental health practitioners to learn more about our services by requesting a demo today.
Read Also: Depression And Anxiety Assessment Test
Diagnostic Criteria For Major Depressive Disorder Dsm
The following criteria, as determined by the DSM-5, must be met in order for a diagnosis of major depressive order to be made:
At least five of the following symptoms must be present during the same 2-week period and represent a change from previous functioning. Additionally, at least one of the symptoms is either a depressed mood or a loss of interest or pleasure.
The diagnostic code for major depressive disorder is based on recurrence of episodes, severity, presence of psychotic features, and status of remission. These codes are as follows:
Severity
- With seasonal pattern
Documentation And Coding: Major Depressive Disorder
Depression is the most common mental disorder. It carries a high cost in terms of relationship problems, family suffering and lost work productivity, according to the American Psychiatry Association . Accurately and completely documenting and coding Major Depressive Disorder can help our members access needed resources. Below is information from the ICD-10-CM Official Guidelines for Coding and Reporting .
Coding for MDD
When coding and documenting for MDD, its critical to capture the episode and severity with the most accurate diagnosis codes.
Documentation should include:
- Severity: mild, moderate, severe without psychotic features or severe with psychotic features
- Clinical status of the current episode: in partial or full remission
The fourth and fifth characters in the ICD-10-CM codes capture the severity and clinical status of the episode.
F32.9 MDD, single episode, unspecified, is equivalent to Depression Not Otherwise Specified , Depressive Disorder NOS and Major Depression NOS. This code should rarely be used and only when nothing else, such as the severity or episode, is known about the disorder.
Best Practices
For more details, see:
|
F33.9 |
Recurrent, unspecified |
Recommended Reading: Major Depressive Disorder Disability Rating
Enhancing Healthcare Team Outcomes
An interdisciplinary approach is essential for the effective and successful treatment of MDD. Primary care physicians and psychiatrists, along with nurses, therapists, social workers, and case managers, form an integral part of these collaborated services. In the majority of cases, PCPs are the first providers to whom individuals with MDD present mostly with somatic complaints. Depression screening in primary care settings is very imperative. The regular screening of the patients using depression rating scales such as PHQ-9 can be very helpful in the early diagnosis and intervention, thus improving the overall outcome of MDD. Psychoeducation plays a significant role in improving patient compliance and medication adherence. Recent evidence also supports that lifestyle modification, including moderate exercises, can help to improve mild-to-moderate depression. Suicide screening at each psychiatric visit can be helpful to lower suicide incidence. Since patients with MDD are at increased risk of suicide, close monitoring, and follow up by mental health workers becomes necessary to ensure safety and compliance with mental health treatment. The involvement of families can further add to a better outcome of the overall mental health treatment. Meta-analyses of randomized trials have shown that depression outcomes are superior when using collaborative care as compared with usual care.
What Are The Symptoms Of Major Depressive Disorder
Your doctor or a mental health professional can diagnose major depressive disorder based on your symptoms, feelings, and behaviors.
Typically, youll be asked specific questions or given a questionnaire so health professionals can better determine whether you have MDD or another condition.
To be diagnosed with MDD, you need to meet the symptom criteria listed in the Diagnostic and Statistical Manual of Mental Disorders, 5th edition . This manual helps medical professionals diagnose mental health conditions.
According to its criteria:
- you must experience a change in your previous functioning
- symptoms must occur for a period of 2 or more weeks
- at least one symptom is either depressed mood or loss of interest or pleasure
You must also experience 5 or more of the following symptoms in the 2-week period:
- You feel sad or irritable most of the day, nearly every day.
- Youre less interested in most activities you once enjoyed.
- You suddenly lose or gain weight or have a change in appetite.
- You have trouble falling asleep or want to sleep more than usual.
- You experience feelings of restlessness.
- You feel unusually tired and have a lack of energy.
- You feel worthless or guilty, often about things that wouldnt usually make you feel that way.
- You have difficulty concentrating, thinking, or making decisions.
- You think about harming yourself or suicide.
Symptoms parents should be aware of in their teens include the following:
Recommended Reading: Lack Of Sleep Causes Depression
Major Depressive Disorder Single Episode In Full Remission
- 2016201720182019202020212022Billable/Specific Code
- F32.5 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
- The 2022 edition of ICD-10-CM F32.5 became effective on October 1, 2021.
- This is the American ICD-10-CM version of F32.5 – other international versions of ICD-10 F32.5 may differ.
- Applicable To annotations, or
Major Depressive Disorder Causes
GENETICS:
If there is a history of Major Depressive Disorder in close family members, and especially in immediate family members , then the risk for a major depressive episode will be three times more likely.
BIOLOGICAL
Biological causes such as levels of serotonin, norepinephrine, and dopamine, can cause depression or other symptoms if levels are low.
Obsession and compulsion due to serotonin deficiency Attention and anxiety with low levels of nor-epinephrine Attention, motivation, and pleasure with low levels of dopamine Other biological factors may include tryptophan deficiency, which the body uses to make serotonin
ENVIRONMENTAL/ PSYCHOLOGICAL
Loss of someone due to death or divorce Sexual or emotional abuse
Risk factors of Major Depressive Disorder
Major Depressive Disorder is not limited to adults and elderly populations. A substantial proportion of patients experience their first episode of major depression during their developmental years.
There are four major risk factors associated with major depression: Gender: major depression is higher in females than males Poor lifestyle Traumatic childhood experience Specific personality traits
Studies in the United States showed an estimation of 17% of the population has experienced or is experiencing major depression. Another study found that nearly 5% of the population reported meeting criteria for major depressive disorder in the last 30 days.
Read Also: How To Help My Teenage Daughter With Depression And Anxiety
Emerging Trends In Substance Misuse:
- MethamphetamineIn 2019, NSDUH data show that approximately 2 million people used methamphetamine in the past year. Approximately 1 million people had a methamphetamine use disorder, which was higher than the percentage in 2016, but similar to the percentages in 2015 and 2018. The National Institute on Drug Abuse Data shows that overdose death rates involving methamphetamine have quadrupled from 2011 to 2017. Frequent meth use is associated with mood disturbances, hallucinations, and paranoia.
- CocaineIn 2019, NSDUH data show an estimated 5.5 million people aged 12 or older were past users of cocaine, including about 778,000 users of crack. The CDC reports that overdose deaths involving have increased by one-third from 2016 to 2017. In the short term, cocaine use can result in increased blood pressure, restlessness, and irritability. In the long term, severe medical complications of cocaine use include heart attacks, seizures, and abdominal pain.
- KratomIn 2019, NSDUH data show that about 825,000 people had used Kratom in the past month. Kratom is a tropical plant that grows naturally in Southeast Asia with leaves that can have psychotropic effects by affecting opioid brain receptors. It is currently unregulated and has risk of abuse and dependence. The National Institute on Drug Abuse reports that health effects of Kratom can include nausea, itching, seizures, and hallucinations.
Resources: