Depression As A Complex Systemic Disease:
Before we dive into the details on mitochondrial dysfunction in depression, Id like to point out that for many people, depression goes hand-in-hand with other chronic diseases, pointing to depression as being a systemic problem in the body. Statistically, depression is linked with the following chronic diseases:
- cardiovascular disease
- Immune system impairment
- cancer
In other words, depression is not all in your head. At least not in the way that the pejorative term implies. Youll notice that most of the chronic diseases linked to depression also involve mitochondrial dysfunction.
Research on depression focused for several decades on neurotransmitter levels, with a focus on serotonin. But serotonin has turned out not to be the problem or solution for many with depression.
A systemic point of view shows that changes in depression can physically alter other tissues as well as change the brain.
Recent research shows that for people with long-term psychiatric illnesses, such as major depressive disorder, bipolar disorder, or schizophrenia, there are structural changes that take place in the brain. For me, the mental image is that neurotransmitters are acting like software, and altering the software code can alter mood. But the structural changes are more like changes to the hardware of the system like switching from a Mac to a Windows PC. Changing the software can alter the user experience , but you are still limited by the hardware change.
Back To Mitochondrial Dysfunction And Depression
I dont want to get too far into the weeds here, so back to the point of this article:
My first thought in reading about mitochondrial dysfunction and depression was how do the researchers know that the mitochondrial dysfunction is causing depression and not the other way around?
The link between mitochondrial dysfunction and depression has been shown in a lot of studies. Lets take a look at a few animal studies as examples:
Adding stress hormones causes mitochondrial dysfunction: The addition of corticosterone in mice will cause depression, and this is one way of making a mouse model of depression. To find out why, researchers tested the liver cells to see what had changed in the depressed mice. The results showed that the changes in gene expression were associated with decreased lipid metabolism and alterations in the genes needed for energy production in the mitochondria.
Adding healthy mitochondria eradicates depression symptoms: Transplanting healthy mitochondria into the brains of mice cures depressive symptoms. In the experiment, the researchers caused depression in mice with lipopolysaccharide . The researchers assessed the depressive symptoms, looked at BNDF and neurogenesis in the brain, and quantified the neuroinflammation and oxidative stress. Injecting healthy mitochondria into the brain was able to reverse all the problems.
Evolutionary Conservation Of Mdd Risk Genes
At an intuitive level, one might imagine that genes causing MDDa disorder of higher brain function affecting extensive neural networks including the limbic systemwould tend to be unique to humans or more prevalent in higher species and absent in simple organisms that lack equivalent brain regions and behavioral complexity. However, based on previous work by our group , we hypothesized that MDD risk genes would be evolutionarily conserved. As summarized in Figure 1, the MDD risk-gene counterparts are highly conserved in C. elegans in comparison to genomic analyses of human genes found in this species. Thus, Kim et al. reported that 60.8% of human genes have an ortholog in C. elegans compared to 82.1% of MDD genes as shown here. Similar conservation of MDD risk genes was observed in zebrafish. Across the entire genome, 71.4% of human genes had an ortholog , whereas 96.4% of MDD genes had a counterpart in this species . These data are consistent with findings of strong conservation of risk genes for schizophrenia and bipolar disorder in these two species. In fact, the degree of conservation of MDD risk genes is midway between that observed in the other two psychiatric disorders.
Recommended Reading: Icd 10 Code For Anxiety And Depression
Generation Scotland: Scottish Family Health Study
The family and population-based Generation Scotland: Scottish Family Health Study cohort12 consisted of 23,960 individuals, of whom 20,195 were genotyped with the Illumina OmniExpress BeadChip . The genotypic data was uploaded to the Michigan Imputation Server36 and phased using SHAPE IT v2.r83737 and imputed using the Haplotype Reference Consortium reference panel 38. The imputation of GS:SFHS has been published previously39. We applied an imputation accuracy threshold of ⥠0.8 and this provided us with a total of 8,633,288 genome-wide variants calls for 20,032 individuals.
Genetic Dataquality Control Snp
Quality control
Participants in the final sample were unrelated and of European ancestries which were identified using a previously described analytical pipeline .
A total of 560,173 genotyped and 9,940,918 imputed SNPs remained after QC. Genotyped SNPs were used to estimate heritabilities and imputed SNPs were used to compute genetic correlations.
SNP-based Heritability
Phenotype-Correlation-Genotype-Correlation was used to estimate the SNP-based heritability of the 32 depression phenotypes . To convert to the liability scale, population prevalence was assumed to equal the sample prevalence prior to the application of any exclusion criteria for each phenotype . As recommended, the major histocompatibility complex region was removed reducing the total number of SNPs used to estimate the SNP-based heritability to 554,059 . The first six genetic principal components, genotyping batch and assessment centre were included as covariates for all phenotypes.
Genetic correlation
Don’t Miss: How To Fight Depression As A Christian
What Is Major Depression
Major depression, also known as unipolar or major depressive disorder , is characterized by a persistent feeling of sadness or a lack of interest in outside stimuli. The unipolar connotes a difference between major depression and , which refers to an oscillating state between depression and mania. Instead, unipolar depression is solely focused on the lows, or the negative emotions and symptoms that you may have experienced.
Fortunately, major depression is well understood in the medical community and is often easily treatable through a combination of medication and talk therapy. Below is a guide to everything from the symptoms and causes of major depression, to statistics and treatment that you can seek from a medical professional if you feel that you need assistance.
Diet And Lifestyle Suggestions:
Dumping the fast-food and junk food: Burning fat increases oxidative stress creation in the mitochondria. In general, a Western diet that includes fried foods, like french fries and chicken nuggets, is going to increase oxidative stress. If you are eating a lot of junk food, this is the first place to target. Cut out the donuts, french fries, and pizza
Increasing folate for MTHFD1L: Increasing folate may help with reducing homocysteine levels for people with MTHFD1L variants. Check out the folate-rich foods and recipes article.
Avoiding BPA: A component of plastics, BPA has recently been shown to induce mitochondrial dysfunction, causing oxidative stress. BPA is also linked to depression and anxiety in children. Read more about BPA, genetics, and avoiding BPA.
Give blood : For some people with high iron, giving blood improves mood. Check your HFE genes for mutations related to hemochromatosis.
Talk with your doctor about ketamine administration: Ketamine administration by a professional rapidly reverses depression for some people. An animal study shows that this is linked to reversing mitochondrial dysfunction. Ketamine in rats reverses the mitochondrial respiratory chain dysfunction seen in a chronic mild stress model of depression.
Read Also: Depression And Anxiety Support Groups Las Vegas
Treating Major Depressive Disorder
While depression is a serious condition, it can be treated. In fact, between 80% to 90% of people with depression respond well to treatment, and almost all patients get some relief from their symptoms.
Its important to seek treatment for depression as soon as possible, because the earlier it is treated, the more effective the treatment can be. Ignoring the symptoms of depression and leaving it untreated can lead to self-harm or death.
Treatment for depression may involve medication, therapy, or brain stimulation. The treatment modalities chosen can depend on the severity of the depression and your individual needs.
Other Causes Of Oxidative Stress:
The gut-brain axis refers to the link between what is going on in the intestines and brain changes Leaky gut causes an increase in bacterial pathogens moving across the gut barrier. This increases inflammatory cytokines and is linked to depression.
An excess of iron can cause an increase in oxidative stress. Research shows that iron accumulation in the brain can cause neuropsychiatric disorders.
The body tightly regulates iron levels and usually only absorbs the right amount from foods. But genetic variants in the HFE gene can increase iron absorption.
Excessive alcohol consumption impacts the mitochondria. When consuming normal, low amounts of alcohol, your cells use the alcohol dehydrogenase enzymes to break it down and eliminate it. But when drinking a lot of alcohol, the body will need the CYP2E1 enzymes. CYP2E1 enzymes work in the mitochondria and endoplasmic reticulum in response to high ethanol levels, and this produces a lot of ROS and oxidative stress.
You May Like: When To Get Help For Postpartum Depression
What Are The Risk Factors For Depression
While genes do play a significant role in depression symptoms, a persons personality traits, and their environment can also cause them to develop the disorder. In cases of postpartum depression, women with no other risk factors for depression can develop symptoms thanks to significant fluctuations in hormone levels, and the stress of giving birth and caring for a newborn. When it comes to major depressive disorder, some of the most significant risk factors for developing the condition include the following:
- Self Criticism and Negativity
Being self-critical or prone to a negative outlook are both inherent personality traits that can increase someones risk of developing major depressive disorder. Researchers from Yale and Wesleyan University found self-criticism was a significant factor in both depression manifestation and problems functioning in relationships. Further studies have uncovered that people with high levels of self-criticism, and feelings of helplessness and separation and rejection anxiety had a high risk of experiencing depressive episodes.
- Trauma
- Major Illness
- Genetics
Depression Genetics And Mitochondrial Function
Depression is a huge, global problem. Estimations show that depression has a lifetime prevalence rate of 20% worldwide. More than 1 million people per year die of suicide. These are startling statistics for a disease that doesnt seem to have enough real solutions. SSRIs work for some people , and these medications reduce the risk of suicide by about 40% in adults .
Obviously, we need better solutions that get to the root of the problem of depressive disorders. For some people, the answers may lie in the tiny powerhouse of the cell: the mitochondria.
In this article, I will explore the research on how mitochondrial dysfunction relates to major depressive disorder. Included will be information on causes of mitochondrial dysfunction as well as genetic variants that link the risk of depression to the mitochondria.
Contents:
Read Also: How Is Depression Different From Feeling Sad
Causes Of Major Depressive Disorder
Depression is caused by an imbalance of chemicals, known as neurotransmitters, in the brain.
Certain genetic, biological, psychological, and environmental factors can increase the chances of someone developing depression however, its important to remember that anyone can develop depression.
The potential causes and risk factors for depression include:
No Depression Gene But Still Genetic Vulnerability

One thing is becoming increasingly clear: Its unlikely that a depression gene exists. The mental health world was hopeful, as having a single gene would make it easy to test people for depression and could lead to medications for effective treatment, too.
All hope isnt lost. While the existence of a single depression gene is doubtful, researchers have made great strides in understanding the connection between genetics and depression. Its known with certainty that numerous genes are involved in depression. Scientists are striving to understand how they work in combination to trigger major depressive disorder.
While there are still many questions, it is becoming increasingly clear that having certain genes makes someone genetically vulnerable to developing depression. Possibly, the more genes linked to depression someone has, the more susceptible they are to the illness.
Recommended Reading: I Feel Depressed And Worthless
Types Of Major Depressive Disorder
You might be surprised to learn that there are many different types of major depressive disorder that can affect you can make living your daily life difficult. Each type often has different causes, but they typically involve the same feeling of disinterest in activities that you once loved and an overall feeling of melancholy. These are divided into subtypes called specifiers that determine how long the diagnosis of depression lasts and the defining characteristic of each type.
Polygenic Risk Score Profiling And Binomial Sign Tests
Each data set was filtered on the basis of statistical imputation information greater than 0.8 and minor allele frequency greater than 0.01 in both CONVERGE and PGC overall linkage disequilibrium -based ‘clumping’ was used to obtain an approximately independent set of SNPs while preferentially retaining the most significant SNP within 500-kb windows. We computed weighted polygenic scores , based on varying P-value thresholds in the ‘training set’ results P-value thresholds ranged between 105 and 0.5. We evaluated the significance of casecontrol differences using logistic regression and covarying ancestry-based principal components and a study indicator variable. The predictive value of these scores is reported in terms of Nagelkerkes pseudo-R2 .
Using the same sets of SNPs and the same P-value thresholds, we applied a binomial sign test to determine whether the number of SNPs demonstrating consistent directions of allelic effects between CONVERGE and PGC was greater than expected by chance .
Also Check: Free Depression Counseling El Paso Tx
Major Depression And Genetics
How common is major depression? At least 10% of people in the U.S. will experience major depressive disorder at some point in their lives. Two times as many women as men experience major depression.
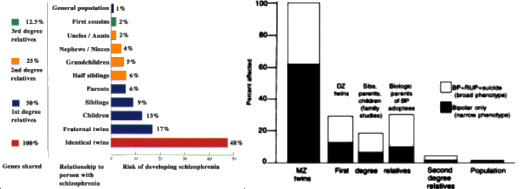
How do we know that genes play a role in causing depression? Scientists look at patterns of illness in families to estimate their heritability, or roughly what percentage of their cause is due to genes. To do this we find people with the disease who have a twin, and then find out whether the twin is also ill. Identical twins share 100% of their genes, while non-identical twins share 50% of their genes. If genes are part of the cause, we expect a patients identical twin to have a much higher risk of disease than a patients non-identical twin. That is the case for major depression. Heritability is probably 40-50%, and might be higher for severe depression.
This could mean that in most cases of depression, around 50% of the cause is genetic, and around 50% is unrelated to genes . Or it could mean that in some cases, the tendency to become depressed is almost completely genetic, and in other cases it is not really genetic at all. We dont know the answer yet.
We can also look at adoption studies, to see whether an adopted persons risk of depression is greater if a biological parent had depression. This also seems to be the case.
However, many people who develop major depression did not have this type of personality before their depression started.
The Role Of Genetics In Depression
As far as researchers know, it’s the interplay of genes and other factors that determine whether someone develops depression.
Some studies have indicated that someone with a first-degree relative diagnosed with depression could be three times more likely to be diagnosed with depression in their lifetime compared to the general population.
However, its important to note that while studies have suggested a clear link within families, these findings dont account for those who develop depression without a family history.
Research has demonstrated that genes play a role in the potential risk for many health conditions, including depression.
Studies have suggested there is a heritable component to depression. Some research has also indicated that women may be more susceptible to the genetic influences associated with depression than men.
Read Also: Latuda For Bipolar 2 Depression
Is Depression Genetic Or Hereditary
Is depression genetic? That is one of the most elusive questions about this complex illness. Many people want to know what causes depression because when we identify a cause, we can target it and block it so we can stop depression long before it starts. Researchers are discovering that, to a limited extent, depression can sometimes be genetic or hereditary.
Currently, there is no definitive answer about the degree to which depression is genetic. This isnt for lack of research. There are two types of ongoing studies: Genome-Wide Association Studies and Gene-Environment Interaction studies . Over 2,000 GWAS studies alone have been undertaken to uncover the genetics behind major depressive disorder. Countless others have attempted to locate a depression gene and solve the mystery of the cause of depression. To date, the exact nature of the genetic link and genes involved hasnt been identified.
This doesnt mean, however, that all these studies have been fruitless. Scientists are learning quite a lot about depression and genetics.
Life Expectancy And The Risk Of Suicide
Depressed individuals have a shorter life expectancy than those without depression, in part because people who are depressed are at risk of dying of suicide. Up to 60% of people who die of suicide have a mood disorder such as major depression, and the risk is especially high if a person has a marked sense of hopelessness or has both depression and borderline personality disorder. About 2â8% of adults with major depression die by suicide, and about 50% of people who die by suicide had depression or another mood disorder. The lifetime risk of suicide associated with a diagnosis of major depression in the US is estimated at 3.4%, which averages two highly disparate figures of almost 7% for men and 1% for women . The estimate is substantially lower than a previously accepted figure of 15%, which had been derived from older studies of people who were hospitalized.
Depressed people have a higher rate of dying from other causes. There is a 1.5- to 2-fold increased risk of cardiovascular disease, independent of other known risk factors, and is itself linked directly or indirectly to risk factors such as smoking and obesity. People with major depression are less likely to follow medical recommendations for treating and preventing cardiovascular disorders, further increasing their risk of medical complications.Cardiologists may not recognize underlying depression that complicates a cardiovascular problem under their care.
Don’t Miss: Do You Have To Be Sad To Have Depression