Brightquest Levels Of Care For Psychotic Depression
Psychotic depression includes a multiplicity of symptoms that take time and special care to treat. At BrightQuest, we tailor our treatment programs to meet each clients unique needs, regardless of the nature or severity of their condition. Our ultimate goal is to help them recover from their mental health struggles, but in a way that equips them with effective coping mechanisms that can prevent future recurrences.
To facilitate thorough and effective healing, we offer different levels of care appropriate for different stages of recovery. The options include:
It can take a year or more to complete a BrightQuest treatment plan, which is a testament to our in-depth approach to recovery. Your loved one will leave our facilities feeling refreshed in mind, body, and spirit, ready to embrace opportunity while living their lives to the fullest.
Distinction Between Psychotic Depression And Schizophrenia
By definition, in both DSM-IV and DSM-V, the psychotic symptoms in major Depressive disorder with psychotic features are episodic and occur only during an episode of major depression. In contrast, patients with schizophrenia exhibit psychotic symptoms that occur in the absence of an identifiable mood disorder. A family history of schizophrenia among relatives is not associated with an increased risk of psychotic depression.26 A few biological markers have been documented that distinguish psychotic depression from schizophrenia. Patients with psychotic depression and schizophrenia differ in hypothalamic-pituitary-adrenal axis activity and all-night sleep electroencephalogram readings.1
A Review Of Psychosis
Etymologically, the term psychosis means “abnormal condition of the soul .” This is most associated with schizophrenia, but psychotic symptoms occur across numerous disorders, as written about in The Many Faces of Psychosis.
While it is the primary feature of diseases in schizophrenia spectrum disorders, we may see delusions, hallucinations, and/or disorganized psychotic symptoms in depression, mania, some personality disorders, PTSD, and even some severe OCD presentations can have delusional material. Psychosis is also present in dementia and delirium.
While sometimes it will be obvious that the patient is experiencing psychosis, like talking to themselves and looking about, in other instances it may be more subtle. Perhaps the patient “has it together enough to know they don’t have it together” and is able to hide it. After all, they’re feeling bad enough being depressed, why would they want to let on that they’re “crazy,” too? This is where the clinician becomes the detective.
First, it is always a good idea to ask any new patient during their diagnostic interview about psychotic symptom experiences, even if it is not a presenting complaint. Cover your bases! Remember, patients don’t necessarily know what hallucinations and delusions are, so don’t point-blank ask, “Have you ever hallucinated or had delusions?”
Read Also: Can Depression Be Cured Without Drugs
Missed Diagnosis Of Psychotic Depression
Data from the National Institute of Mental Health Study of the Pharmacotherapy of Psychotic Depression 2 indicates that clinicians frequently miss the diagnosis of psychotic depression, in large part, due to a lack of recognition of the psychotic features. In the STOP-PD Study, 27% of 130 diagnoses among a well-characterized sample of patients with a research diagnosis of psychotic depression were initially incorrectly diagnosed. It is likely that the missed diagnosis rate observed in this study was a conservative estimate of the rate in the general clinical population because patients with comorbid conditions such as a history of substance abuse in the past 3 months or unstable medical conditions were excluded. Psychotic depression was most commonly misdiagnosed as major depressive disorder without psychotic features, depression not otherwise specified , or mood disorder NOS. It was quite striking that none of the patients with missed diagnoses were considered to have a psychotic disorder. This finding suggests that the clinicians were missing the psychosis rather than the mood disorder.
Major Depression With Psychotic Features Treatment
Antidopaminergic Therapy for Managing Comorbidities in Patients with Parkinsons Disease Treatment may not be necessary when psychotic symptoms are not troublesome.
which usually results in a worsening of the parkinsonian features and may be poorly tolerated. It is recommended.
Depressive disorders can be serious, disabling illnesses. Major depressive disorder ,1 defined as the presence of depressed mood or loss of interest or.
In addition to the challenge of differentiating mania and psychotic depression from schizophrenia.
or at least a gene of major effect. It is possible that a common gene polymorphism will.
What Helps For Major Depression What you should know about infertility and depression Nigerians urged to help less privileged My brother. The economy of the country is a major factor. There is poverty in the land and. Researchers explored the neurobiology related to reward-based reinforcement learning and psychomotor retardation in patients in remission from MDD. Experts say the number of
Abstract & Introduction Diagnostic Concepts and Differential Diagnosis Treatment Conclusion References.
complex disorders with transient psychotic features that do not neatly correspond to.
or when psychotic or melancholic features are prominent. With proper treatment, the prognosis and outcome for chronic depression should remain optimistic. Antidepressant Medicines. Overview of the.
Efficacy in mania or in acute psychotic reactions is at least as.
These features.
Don’t Miss: Is There A Medication That Treats Both Depression And Pain
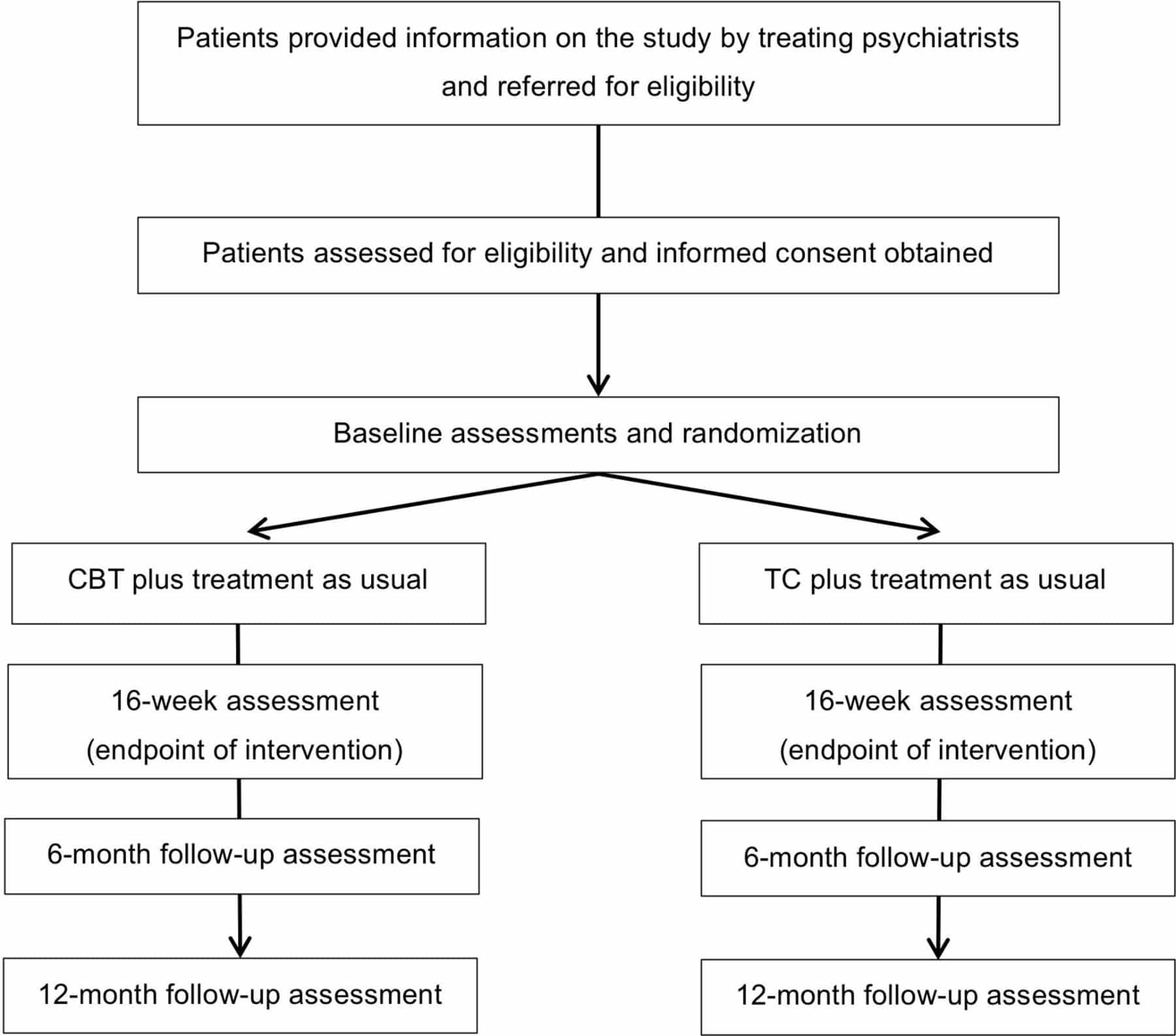
Hypotheses And Exploratory Aims
Primary hypothesis
H1.The combination of sertraline and olanzapine will be associated with less risk of relapse than the combination of sertraline and placebo.
Secondary hypotheses
H2. The combination of sertraline and olanzapine will be associated with higher weight, higher total cholesterol, and higher triglycerides compared with the combination of sertraline and placebo in the randomized phase.
H3. Older age will be associated with less weight gain than younger age during the open-label phase.
Exploratory aims
i) Explore older age as a moderator of change in weight, lipids, and insulin resistance during the randomized phase. ii) Explore the association of selected genetic polymorphisms with: a) response, b) relapse, and c) weight, lipids, and insulin resistance during the open-label and randomized phases of the study.
Causes Of Schizoaffective Disorder
Scientists donât know the exact cause. Risk factors for schizoaffective disorder include:
- Genetics: You may inherit a tendency to get features linked to schizoaffective disorder from your parents.
- Brain chemistry and structure: If you have schizophrenia and mood disorders, you might have problems with brain circuits that manage mood and thinking. Schizophrenia is also tied to lower levels of dopamine, a brain chemical that also helps manage these tasks.
- Environment: Some scientists think things like viral infections or highly stressful situations could play a part in getting schizoaffective disorder if youâre at risk for it. How that happens isnât clear.
- Drug use: Taking mind-altering drugs.
Schizoaffective disorder usually begins in the late teen years or early adulthood, often between ages 16 and 30. It seems to happen slightly more often in women than in men. Its rare in children.
Because schizoaffective disorder combines symptoms that reflect two mental illnesses, itâs easily confused with other psychotic or mood disorders. Some doctors may diagnose schizophrenia. Others may think itâs a mood disorder. As a result, itâs hard to know how many people actually have schizoaffective disorder. Itâs probably less common than either schizophrenia or mood disorders alone.
Read Also: Why Am I Depressed When I M Alone
How Do You Know If Youre Having A Nervous Breakdown
“Nervous breakdown” is not a medical term, but it is often used colloquially to mean intense mental and emotional distress.
In terms of major depressive disorder, symptoms of psychosis, including hallucinations and delusions, can occur. When this happens, it is called MDD with psychotic features, or psychotic depression.
Psychotic Depression Vs Schizophrenia
The major diagnostic distinction between psychotic depression and schizophrenia is that with psychotic depression the psychosis occurs at the same time as major depressive episodes, while the psychosis due to schizophrenia generally occurs without a mood disorder, such as depression, being present. It also is accompanied by other symptoms and functional difficulties.
Don’t Miss: How To Cope With Chronic Depression
Learn More About Depression In The Elderly
Depression can occur in the elderly, but it is not a normal part of aging. Find out more about depression in the elderly here.
Psychotic depression is taken very seriously by mental health professionals because the individual suffering from it is at an increased risk of self-harm.
The suicide rate in people with psychotic depression, when they are ill and in their acute phase, is much higher than it is with major depression, says Anthony J. Rothschild, MD, the Irving S. and Betty Brudnick Endowed Chair, Professor of Psychiatry at the University of Massachusetts Medical School in Worcester, Massachusetts and the author of the Clinical Manual for the Diagnosis and Treatment of Psychotic Depression.
Its important to distinguish psychotic depression from psychosis as well as schizophrenia, experts say. Psychosis by itself is not a disease, explains Timothy B. Sullivan, MD, chair of Psychiatry and Behavioral Sciences at Staten Island University Hospital in Staten Island, New York. Its not an illness in itself, just as fever is not an illness, he explains. Psychosis is caused by an impairment in the part of the brain that helps us discern what is happening internally versus what is happening externally.
Also Check: Vitamin D For Seasonal Depression
What Are The Symptoms Of Mood Disorders
Each mood disorder has different symptoms and/or different patterns of symptoms.
Mood disorders typically have symptoms that affect your mood, sleep, eating behaviors, energy level and thinking abilities .
In general, depressive symptoms include:
- Feeling sad most of the time or nearly every day.
- A lack of energy or feeling sluggish.
- Feeling worthless or hopeless.
Also Check: Fun Activities To Help With Depression
Treatment Of Major Depression With Psychotic Features
Psychotic depression, also known as major depressive disorder with psychotic features, is a serious condition that requires immediate treatment and close monitoring by a medical or mental health professional. Major depressive disorder is a common mental disorder that can negatively affect many areas of someones life. It impacts mood and behavior as.
nosed as major depressive episode, severe with. stays for clinical treatment and research has resulted. psychotic features the psychotic.
estimate that psychotic features are present in 1419% of.
Major depression Psychosis Cognitive behavior therapy.
Major depressive disorder is a mental health condition that affects more than 16 million adults every year. A.
Psychotic features within major depressive disorder are associated with poor treatment outcome. This article explores whether sociodemographic and.
history of any psychotic disorder or psychotic features, or any personality disorder of sufficient severity to interfere with participation in the study. Other exclusion criteria included a.
He treats children and adults with mood disorders , behavioral problems related to autism spectrum and other developmental disorders, ADHD, anxiety, psychotic disorders.
A careful history and physical examination remain vital components in the approach to late-life individuals with paranoia. Particular attention should be paid to a thorough review of recent.
May 1, 2022.
is a common treatment option for prostate.
Treatment Implications Of Psychotic Features
Clearly, the presence of delusions and/or hallucinations brings additional, significant challenges to treatment. If a patient indeed has a history of psychosis while depressed, it is essential to inquire about the symptoms each session. It is not unusual for psychotically-depressed patients to require hospitalization, which you, as therapist, may be instrumental in organizing if they begin to present a heightened risk to self or others.
Even if a patient isn’t psychotic at the moment, knowing if they have a history of becoming psychotic when depressed is important. At the first sign a depressive episode is setting in, it is a good time to encourage a visit to their psychiatrist to assess for use of an antipsychotic medication to augment their antidepressant, for example. In extreme cases, electroconvulsive therapy , which is explored more fully in an upcoming post in this series on melancholic features, may be necessary . Ideally, we also will incorporate their family/friends by educating them on signs and having the patient agree to let them notify providers of concerns.
The next post on Thursday, Oct. 7, 2021, will feature the anxious distress specifier, another addition to MDD that is correlated to a higher risk of self-harm.
References
Rothschild, AJ. . Challenges in the treatment of major depressive disorder with psychotic features. Schizophrenia Bulletin, 39, 787â796. .
Also Check: How To Get Disability In California For Depression
Identifying And Understanding Major Depression Subtypes
- Psychotic features are present in approximately 20% of major depressive episodes.
- These psychotic symptoms only occur while the person is depressed.
- Common psychotic symptoms in depression include voices saying negative things or delusions of not being sure if they are alive or dead.
In the previous post, readers were reacquainted with the basics of major depressive disorder . Today, we will start looking at the subtypes, beginning with major depression with psychotic features. This means that, while depressed, the person experiences hallucinations/delusions.
Estimates vary, but psychotic depression seems to be present in upwards of 20% of MDD patients and brings some challenges to treatment. Unfortunately, psychotic features are correlated with worse prognosis and morbidity, yet according to a top researcher on the topic, often go unrecognized .
Diagnostic Considerations In Major Depressive Disorder With Psychotic Features
Investigators highlighted the need for adequate diagnosis of psychotic features in patients with major depressive disorder during routine clinical care, according to study findings published in Journal of Clinical Psychiatry1
Patients with MDD may present with psychotic features, including hallucinations and delusions. In these patients, neurobiologic findings, clinical characteristics, family medical history, and treatment response patterns have been reported to differ significantly from patients with non-psychotic MDD.2-8
This observational, cross-sectional study included 1410 adults 18 years and older who met the criteria for MDD9 and had received treatment from one of ten European tertiary centersbetween 2011 and 2016. Investigators evaluated the presence of psychotic features using the Mini-International Neuropsychiatric Interview. Using various rating scales, specialists from the referral centers collected clinical, pharmacologic, and sociodemographic data from participants. The investigators examined the association between these variables and the occurrence of psychotic features using binary logistic regressions.
References
Recommended Reading: What Is Interpersonal Therapy For Depression
A Difference In Treatment Styles
Why is it so important to know the differences between schizoaffective disorder vs schizophrenia? One reason is that both disorders require different approaches to treatment. Treating people for one condition when they suffer from the other does little to help.
For schizophrenia, most treatment revolves around antipsychotic medications, such as chlorpromazine and haloperidol. Schizoaffective disorder treatment also relies on antipsychotics, but the most common one that doctors prescribe is Paliperidone. In fact, its the only FDA-approved drug for this disorder.
With that said, there are some similarities in treatment as well. For example, attending therapy while taking appropriate medication is essential. Therapy can help people work through other issues that accompany these disorders. However, it isnt enough on its own, so they still have to take medication.
Mood Congruent And Mood Incongruent Psychotic Symptoms
The diagnostic and prognostic importance of mood congruent and mood incongruent psychotic symptoms in mood disorders is the subject of ongoing discussion. Some investigators propose that mood incongruent psychotic features indicate a distinct subtype of psychotic depression with a worse prognosis regardless of the severity of depression . This point of view appeared to be supported by a finding that mood incongruent psychotic features aggregated in families and predicted a more severe course . In the Research Diagnostic Criteria, mood disorders with mood incongruent psychotic symptoms are grouped under schizoaffective disorder, based on the concept that mood incongruence conveys a worse course of mood disorders . On the other hand, there is considerable heterogeneity of outcome in these patients .
Regardless of how psychosis is categorized, the bulk of evidence suggests that there is no difference in outcome between psychotic depression with mood congruent versus mood incongruent symptoms . One point about which there is growing consensus is that mood incongruent psychotic symptoms convey greater likelihood of bipolar than unipolar depression .
You May Like: Uv Light Therapy For Depression
What Are The Signs And Symptoms
Major depression symptoms vary from person to person. To receive a diagnosis of major depressive disorder, some of these signs and symptoms must be present for at least two weeks. Anyone who has questions should consult their doctor.
- Continued feelings of sadness, hopelessness, pessimism, emptiness
- Fatigue, lack of energy
- Insomnia or other sleep issues such as waking up very early or sleeping too much
- Anxiety, irritability, restlessness
- Lack of interest or joy in hobbies and activities
- Changes in appetite, leading to weight loss or weight gain
- Moving, talking, or thinking more slowly
- Trouble concentrating, thinking clearly, or making decisions
- Vague aches and pains, such as headaches, joint pain, back pain, or digestive problems
- Thoughts of death or suicide, or suicide attempts
Bipolar With Psychotic Features
Psychosis describes a disconnect from reality, a state of mind where you have trouble recognizing whats real and what isnt. In terms of bipolar disorder, psychosis mainly refers to hallucinations or delusions.
Other key symptoms of psychosis, such as changes in sleep patterns or problems with concentration, can seem very similar to those that characterize mood episodes.
Bipolar psychosis might involve:
These symptoms can be mood congruent, meaning theyre consistent with your other symptoms. They can also be mood incongruent, or inconsistent with your other symptoms. Believing you have superpowers during an episode of depression, for example, would be considered mood-incongruent psychosis.
Psychosis can happen during both manic and depressive episodes. An episode of hypomania that involves psychosis automatically meets the criteria for mania.
You May Like: Will I Be Depressed My Whole Life
Read Also: Depression While Pregnant With Twins
What Medications Treat Schizoaffective Disorder
The provider will figure out the right medicine based on the type of mood disorder the person has:
- Antipsychotics: This is the primary medicine used to treat the psychotic symptoms that come with schizophrenia for example, delusions, hallucinations and disordered thinking.
- Antidepressants: An antidepressant or mood stabilizer such as lithium can help treat mood-related symptoms. Sometimes, a person needs both an antidepressant and an antipsychotic.